In 2000, Millie Shinn developed an ulcer on her right heel. A complication of Shinn’s Type 1 diabetes, the ulcer continued to grow, requiring Shinn to seek treatment and ultimately, a heel reconstruction.
When that did not heal properly, she said she knew amputation was a possibility, though she wasn’t willing to accept it yet. Fast forward to February of 2002 and Shinn was still in bandages from the surgery. After a trip to the Emergency Department, Shinn met with her doctors and they decided it was time to amputate her right leg below the knee.
“My husband was with me and even the nurse that was taking care of me, we were all just bawling before the surgery,” Shinn said of her experience before her first amputation at Vidant Medical Center (VMC). “It was not something that I thought would happen to me … I really wasn’t sure what to expect.”

She said she was motivated after her first surgery to get moving and was lucky to have the opportunity to use an early post-operative prosthesis, or EPOP, which helped her to get out of bed and moving around on a prosthetic limb sooner than she would have without one.
The EPOP was used while she was still healing and about three months after her first surgery, she was fitted with a permanent prosthetic limb. In September of the same year, ulcers began to show up on her left foot. She knew right away how it would end.
She asked what her options were and her providers told her they could continue to clean her ulcers and try to heal her foot for as long as possible. But she told the doctors to move ahead with amputation again.
“I said, ‘I’ve done fine with one fake leg, I’ll be fine with two.’ And that’s what we did,” Shinn said. “It was not circulation issues, it was nerve issues. Circulation was always good I just didn’t have any feeling and had lots of nerve damage.”
Her left leg amputation was also a below-the-knee amputation and she said, like her first amputation, she recovered quickly. Since she knew what to expect the second time around it was not as traumatic an experience—for her. It wasn’t as easy for her son to accept, and at that time, there was not an amputee support group in eastern North Carolina.
Eastern North Carolina Amputee Support Group
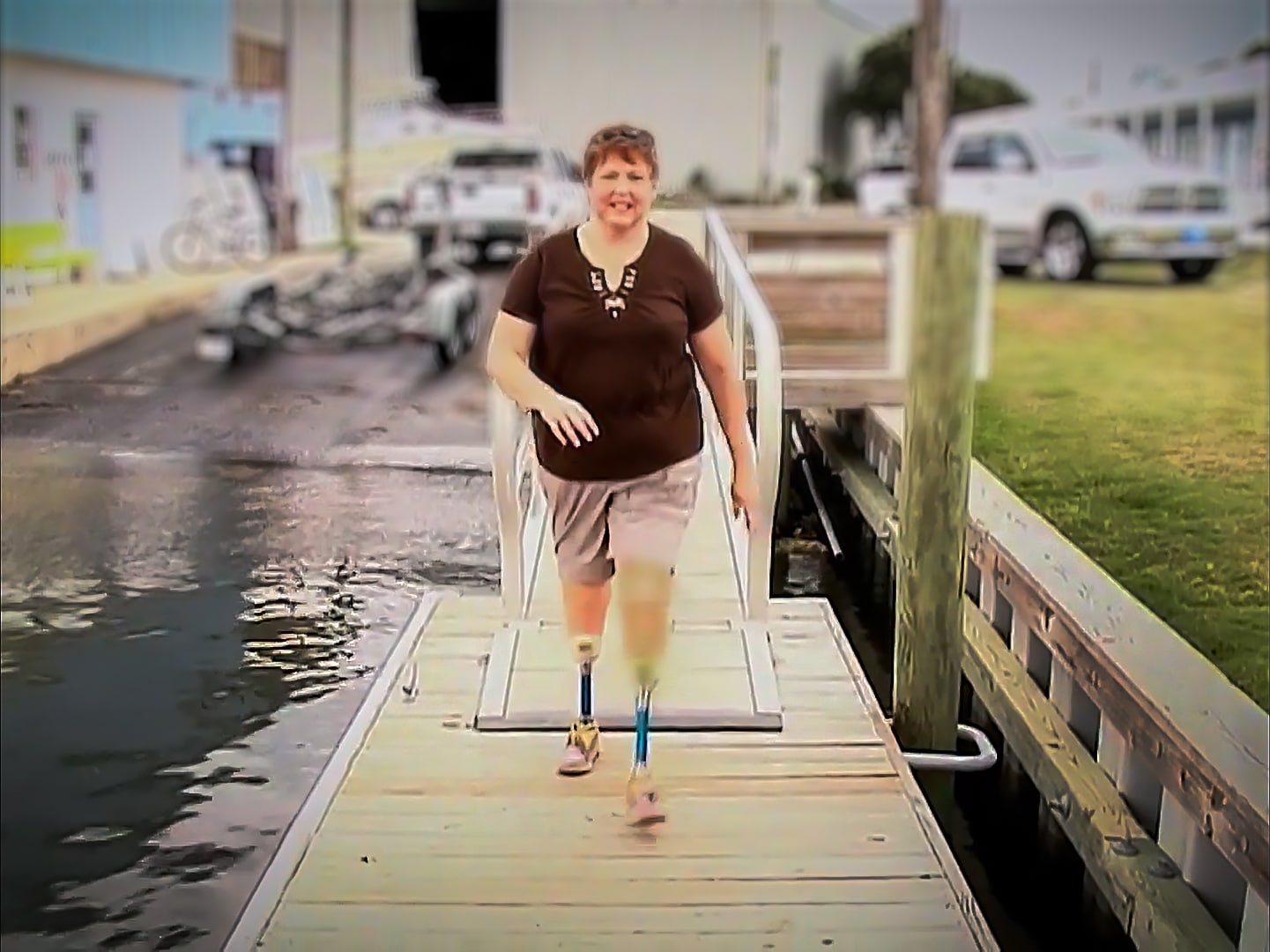
Vidant’s amputee support group, officially called Eastern North Carolina Amputee Support Group, came together for the first time in March of 2006 thanks in large part to Shinn and Helen Houston, an occupational therapy clinical specialist at Vidant Medical Center.
Shinn, who lives nearly two hours away from Greenville and made the drive monthly to help lead the support group, said the first meeting had about eight people. The numbers and traditions have grown along the way, and 16 years later the group continues to meet. COVID-19 means they connect virtually on the third Monday of each month from 4:30 to 5:30 p.m.
Shinn said she estimates that nearly 500 people have joined a meeting a one time or another. She has seen the importance of the meetings for her fellow amputees, especially those in the early stages.
“I think it’s very important because they can see us and realize that there is a life afterwards,” Shinn said. “Yes, it has changed my life and yes this is like a death in your family and a death to you because you’ve actually lost a part of yourself. It’s going to be a part of your life, but it doesn’t have to be a controlling part of your life.”
Houston said she has loved her time participating in the group and looks forward to the meeting each month and interacting with people she now considers family. Houston has also helped lead the group since its inception.
She said the conversations each month are inspiring to her and a reminder of why she chose a career in therapy.
“It’s my responsibility, together with recreational therapy, to bring the people that have had recent amputations and are in rehab right now to the group,” Houston said. “We let them see other people that are a little further along than them and let them ask questions. I can answer their questions all day, but I have two legs, so my experience carries limited weight.”
The group frequently has guest speakers including doctors, massage therapists, highway patrol officers, politicians and prosthetists. Shinn said sometimes people will join the group just once to get a few answers to questions that they have and will not return, but she said that as long as people are getting the help they need, the group feels like it is doing its job.
Houston and Shinn both recalled how meaningful it is to include caregivers, family and friends of amputees in the support group sessions. They even shared that in a few cases, after an amputee has passed, spouses and friends continue to attend the sessions to share their insights and past experiences with the group.
“It’s really neat and it’s become like a family,” Houston said. “For me, who is from South Africa, and who doesn’t have family here, to see the same people every month for 16 years, they know me better than I know myself. We’ve been through all kinds of stuff together.”
Occupational Therapy Month
Along with Limb Loss and Limb Difference Awareness Month, April is also Occupational Therapy Month. While occupational therapists play crucial roles in many areas across the health system, supporting amputees is a special responsibility.
Houston said in the acute care setting, occupational therapists are often the first people helping to get amputees out of bed. From there, it’s about teaching patients how to do all the things they are used to doing, but in a different way. This includes bathing, dressing, grooming, transferring to and from a toilet, and to and from a tub.
She said patients typically need three months for their wounds to heal and their residual limb to be shaped, before they get a prosthetic limb. They would initially be at a wheelchair level—or wheelchair and walker level—for some time during their recovery.
“In inpatient rehab, amputees practice self-care tasks, but they also address what we call instrumental activities of daily living,” Houston said. “That is not just self-care but also taking care of the things in your environment. So that would be things like cooking, grocery shopping, money management, medication management, yardwork and starting to access the community, including returning to driving.”
She described the stages after this as getting people back to doing whatever occupied their time before their amputation and educating them on different ways to do so. Houston mentioned a study of healthy adults that showed it takes at least two days to regain strength from each day spent lying in bed.
“That’s for someone who has not had surgery and has not had anything wrong with them,” Houston said. “So here at Vidant we help to get patients up the day after surgery. You’re trying to prevent blood clots, and help them mentally adjust to their new life. The longer you lay there and are fearful of ‘How am I going to get up and how am I going to do this?’ the bigger the mountain seems.”
Houston said her experiences with amputees are often the most inspiring.
“It’s really neat. It’s an honor to be part of their journey,” Houston said. “To be a part of one of the patient’s hardest times in their lives and be able to support them and show them a little further down the road, makes coming to work every day extremely rewarding. To be able to show them that they’re not the only ones in their current situation and to help them to problem solve how they’re able to get back to doing whatever is important to them – that is why I became an occupational therapist.”