KENANSVILLE – You could say Jon Kornegay was born to be a rural doctor. His father was a physician in a small town in Duplin County in eastern North Carolina. His mother was a graduate of East Carolina University’s first nurse practitioner class in 1976.
But it was his experience at ECU’s Brody School of Medicine that sealed the deal.
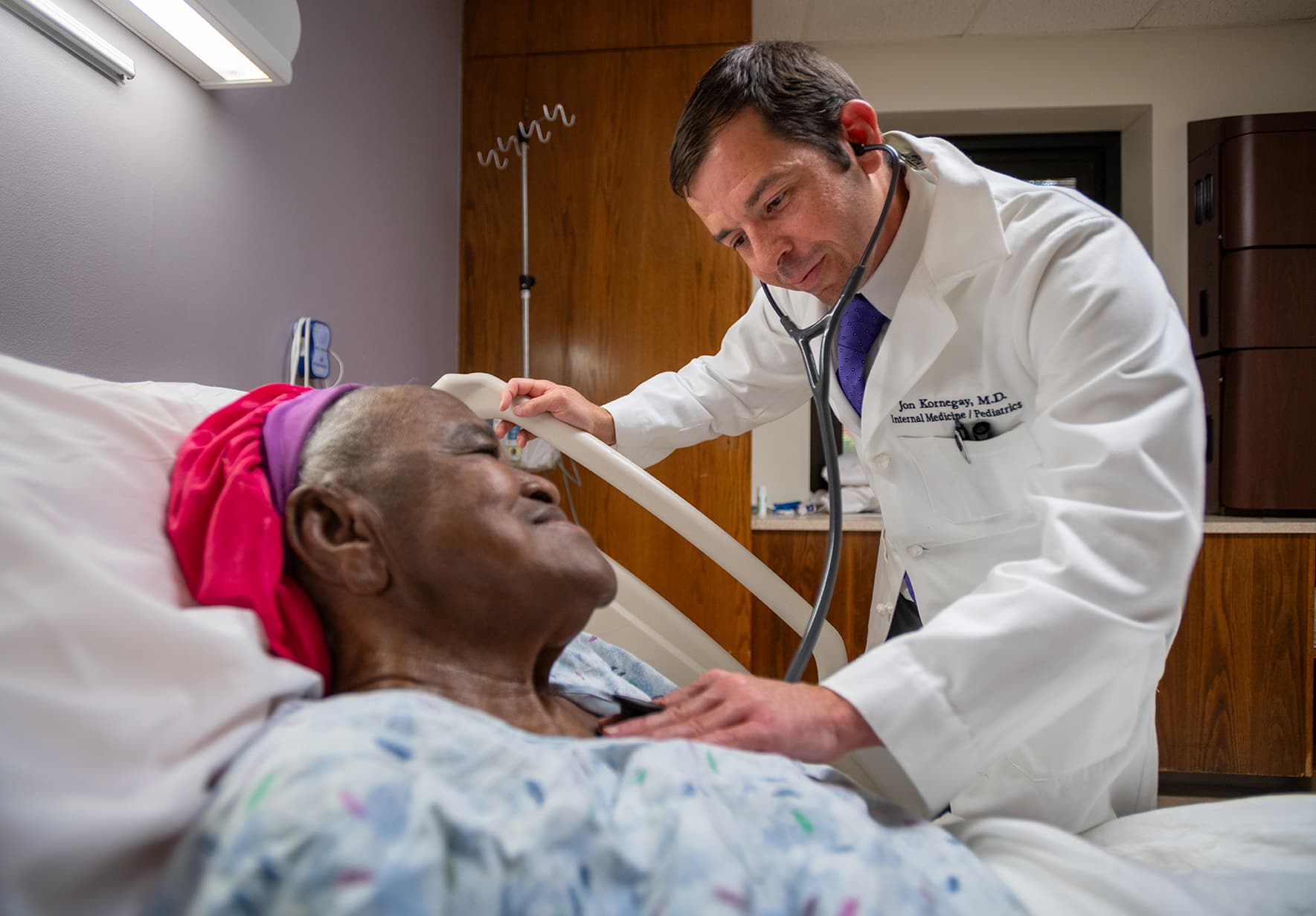
“Even early on in my medical school I saw the emphasis on service. You see other members (at the school), attending physicians and professors, who live that life and lives of service,” he said recently during a break from his job as a hospitalist at ECU Health Duplin Hospital in Kenansville. “Then you get exposed early on to underserved areas and populations and see how rewarding that can be.”
ECU’s medical school was established in 1974 after successfully making the argument – contentious at the time – that it could fill a need in North Carolina to train more primary-care physicians, rather than medical specialists, and find more doctors willing to serve in places like Kenansville.
Since then it has made good on that promise: according to the American Academy of Family Physicians, Brody ranks second in the nation among medical schools in the percentage of family physicians it graduates. The school admits 86 students to each class, all from North Carolina; this year, 52% of Brody’s graduates entered primary-care residencies.
“Developing great primary-care providers for rural areas is at the core of what we do at Brody and within ECU Health,” says Dr. Michael Waldrum, dean of Brody and CEO of ECU Health. “We have students, professors, residents and doctors who really understand that side of health care, and their work in that space leaves a legacy that we can all be proud of.”
A reliable supply of physicians and medical professionals is a critical part of the economy of any rural community:
- Having primary care close to home means residents are more likely to seek treatment for medical problems before they become crises and less likely to have to leave home to get treatment, resulting in fewer missed days of work and better quality of life;
- A healthy medical community is an important selling point for developers recruiting new businesses and for families trying to decide where to move;
- Rural hospitals are among the biggest employers in a county; since 2005, 12 rural hospitals have closed across the state, part of a troubling national trend;
- And medical professionals contribute in other ways. Kornegay also serves as the county’s EMS medical director; one of his colleagues also serves as county health director; other medical professionals serve on chambers, chair charitable boards, and coach sports teams.
Kornegay knows work in rural health care is not for everyone: Physicians can generally make more in cities in highly specialized fields; rural areas don’t offer the same amenities. Overcoming those barriers, he says, will require a variety of approaches, including improved salaries, help with loan repayment, retention bonuses and Medicaid expansion.
But in the meantime, Kornegay finds some people fall in love with work in rural areas, for the quality of life, the chance to get to know patients and neighbors in a deeper way, and for the opportunity to solve a wide range of health concerns.
Kornegay, certified as both an internist and a pediatrician, will often move from a geriatric patient in an ICU to a newborn down the hall.
“If you can get doctors into rural settings for a little while – get to know the environment, get to build their social network, get that experience … you have a chance to keep ‘em,” he says.
Something’s working in Duplin County. All five full-time physicians in Kornegay’s group at Duplin Hospital either went to med school or did their residency at Brody. They join a cadre of other ECU grads in health care and other fields who put down roots in the county.
“There’s a lot of purple and gold here,” says Kornegay. “That’s for sure.”
Further reading on Higher Ed Works
“Eastern North Carolina needs us”: The economic impact of ECU