Valorie Nelson, HIMS operations specialist, joined what was then Pitt County Memorial Hospital in 1981 as a high school student. While her first job was as a volunteer, she has made a few career shifts along the way.
“You could say the hospital and I have grown up together,” she said. “After being a candy striper, I worked in dietary for a while, but I wanted to do more.”
A turning point
Nelson said the support of Dr. Murray Merner, who worked in behavioral health, started her on a new path.
“He gave me this test with abstract questions, and at the end it told you about your strengths and your weaknesses, and it listed some recommended occupations. Dr. Merner said I wasn’t challenged enough and that test helped guide me in a positive direction.”

At that time, Nelson said the hospital offered free classes on-site for team members to progress in their careers.
“You could complete your GED,” she explained. “And they had other classes like basic medical terminology or anatomy and physiology. They weren’t for college credit, but they helped team members excel in the hospital. I took as many as I could, and I did well.”
One of the instructors happened to be a medical records manager, who approached Nelson about a job.
“She asked me what I planned to do after taking the classes, and then offered me a position in medical records,” she said. “I tried to be calm but I was so excited. I knew I wanted a change and I dove in.”
Nelson said she’s had great colleagues and leadership, and she has found her work to remain challenging and interesting.
“Time has a way of going by so quickly, but I’ve been able to advance my career. You have to know that systems are always evolving, and you have to evolve with them,” she said. “Every time I’ve seen an opportunity, I’ve taken it – no one will give it to you. You have to seek it out.”
“When I joined medical records, I didn’t know how to operate the computer,” Nelson continued. “Someone had to show me. From there, I just leaned into it. As systems changed, IS sent a manual and I’d sit down and read it. Then I’d take out a pen and paper and simplify it, creating my own breadcrumbs. You have to be flexible and learn because otherwise you can’t get the work done.”
Looking ahead
Although she recognizes that 45 years is a milestone anniversary, retirement isn’t in Nelson’s immediate future.
“I enjoy what I do – that’s why I’ve been here so long,” she said. “There’s a lot of opportunity in Greenville, but I’ve never found anything that makes me want to leave. I’m proud of what I’ve accomplished and I’m grateful. I don’t take my job for granted.”
She does, however, plan to travel.
“I went to Las Vegas recently, and my favorite place to go is the Dominican Republic,” she shared. “My goal is to get to Europe and see the Eiffel Tower and go to Rome.”
For those just starting their careers at ECU Health, Valorie had some advice.
“It’s our job to bring the light. Don’t come to work expecting others to make you have a good day,” she said.
“Have an open mind,” she added. “You never know what you might learn or who you might meet who will change your life. It’s a life changing place.”
When Ashley Dunn, a quality nurse specialist on the ECU Health Medical Center patient safety team, graduated from nursing school in 2008, she found a place in Pitt County Memorial Hospital’s labor and delivery unit. She loved her team and her work, but in 2014 she was sidelined with an unexpected diagnosis.
“I found out I had cystic fibrosis, which I was not expecting. That took me away from the bedside, so I worked in outpatient case management with Access East until 2016.”
Ashley then switched to working in the post anesthesia care unit (PACU), but the pandemic required another change.
“My doctors did not want me anywhere near the bedside, but I still wanted to work with the hospital. That’s when I found this role in patient safety. Everything fell into place like it was meant to be.”

An unexpected journey
Around the same time she joined ECU Health, Ashley and her husband, David, also wanted to grow their family. Despite polycystic ovary syndrome (PCOS), her cystic fibrosis diagnosis and the everyday stress of life and work, Ashley said she and David assumed things would work out.
“Nothing was happening,” she said. “We didn’t feel pressed to do IVF early on, but then suddenly I was 37 and we felt like we were running out of time.”
Ashley and David underwent IVF and over the next couple of years, she had three embryo transfers.
During that time, she needed multiple testing modalities and a surgery to improve her chances.
“Three transfers didn’t work, and we had one left,” she said. “We said this is it, the last chance, so we threw everything but the kitchen sink at it to make it work. And that last embryo stuck.”
Once pregnant, Ashley said she was doing well until she started leaking amniotic fluid at 28 weeks.
A strong start
“It was a Wednesday and I went to the hospital, knowing I wouldn’t be coming out without a baby,” she said. “I wasn’t in active labor, so they hoped I could get to 34 weeks. Just in case, they gave me steroid shots and magnesium to prevent complications.”
By that Saturday, however, Ashley began feeling mild contractions. They progressed throughout the day, until by that evening, Rhys Dunn was born at two pounds, 14 ounces.
“He came out kicking and screaming,” she laughed.
Rhys was born a fighter, but at 28 weeks, he needed to go to the neonatal intensive care unit (NICU) at James and Connie Maynard Children’s Hospital. This was challenging, especially when it was time for Ashley to discharge home.
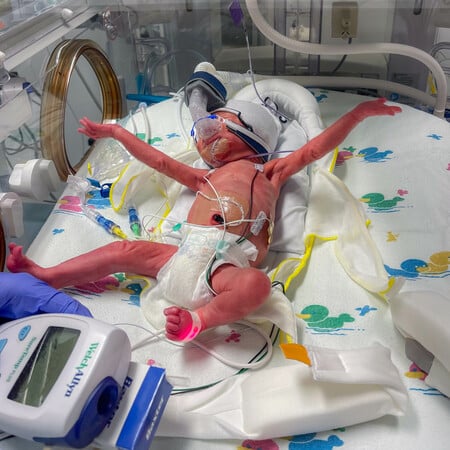
“It’s so hard to leave the hospital without your baby,” she said. “There was a lot of back and forth for us. But we felt at peace about him being there because we had a team that knew what it was doing and cared about us.”
There was even a camera set up so Ashley and David could check on Rhys anytime of the day or night, and the staff were available by phone if they wanted to call for an update on Rhys’s status.
“The nurses were so attentive; the doctors were great. A speech therapist helped him with his feeding. The care partners and the volunteers were helpful,” she said. “The team in labor and delivery were supportive and checked in on us. We felt Rhys was well taken care of, and when he came home, he was ready.”
After 71 days in the NICU, Rhys went home on Father’s Day weekend, and now, he is a happy one-year-old.
“He’s hit all his milestones and he’s very much a happy baby,” Ashley said. He’s sweet as pie, and he brings us so much joy. We have been so blessed.”
Ashley emphasized that she and her family are fortunate to live close to the Maynard Children’s Hospital and the high-quality care they provide.
“I was in a NICU support group and so many parents had to drive two or three hours to see their babies. How lucky we are to have a NICU in our backyard,” she said. “To have that quality of care so close is a luxury.”
The whole experience was a “whirlwind,” but Ashley said it’s been worth it.
“The life we have now wouldn’t be possible without the hospital and the people working there,” she said. “We are so thankful to each and every person.”
Share your story with us at go.ecuhealth.org/gratitude. Stories like these show the lasting impact of the Maynard Children’s Hospital.
As a child, Jennifer Giordano, Cancer Center outreach coordinator, was deeply impressed with nurses.
“I always wanted to be a nurse,” she said. “When I went to the doctor, the nurses were warm and kind, but also steady and wise. I wanted to be that person when I grew up.”
Giordano has indeed been that person during her nearly 30 years as a nurse and 34 years with ECU Health. The Beaufort County native switched from the bedside to community outreach a decade ago, and the change was a good fit.
“It’s great to be on the front end of disease and cancer care and help navigate our patients towards cancer screenings,” she said. “We make a difference, because early detection is key.”
Expanding early detection
In her role, Giordano has been a part of many initiatives that provide education and resources for individuals at risk for cancer.
“We do pop-ups for PSA blood tests for prostate cancer, and last year we screened 22 high-risk individuals,” she shared. “We distribute kits to test for colorectal cancer, perform skin cancer screenings, and run a breast clinic for uninsured patients. It’s a great gig.”

Giordano also works closely with the Lung Cancer Initiative (LCI), a North Carolina organization that connects lung cancer patients and their loved ones with the medical and research community, fuels research, furthers education and supports access to cancer care.
Giordano leads monthly, low-dose CT lung cancer scan clinics for under and uninsured patients, and she also serves on the LCI’s Early Detection Advisory Committee, where she is a champion for the Screening Saves Lives program.
For her work with the LCI, she was recently recognized as the 2025 Dr. Jennifer Garst Healthcare Professional of the Year. The award honors a health care professional who goes above and beyond in providing supportive, patient-centered care, which the LCI said Jennifer “exemplifies . . . in every aspect of her work.”
Why the work matters
Winning the award was humbling and surprising, Giordano said, but it was also deeply personal.
“My dad was a single father, and he started smoking when he was 12,” she explained. “He’s a gifted artist and a talented musician – he’s so much more than a smoker. In 2016, he called me and said something was wrong. We made an appointment with his primary care physician, and they discovered a tumor in the right upper lobe of his lung.”
Giordano’s father underwent chemotherapy and radiation due to the location of his tumor. During that process, his physicians discovered a significant aortic valve stenosis that, once his cancer treatment was complete, required a transcatheter aortic valve replacement. At 79, he’s now doing well, but seeing her father go through cancer treatment gave Jennifer a different perspective.
“Smokers are often blamed for their outcomes, and you can hear it in patients’ voices that they are shaming themselves,” she said. “My dad did that too. He waited a long time to be seen by a doctor, and we all know cancer is easier to treat if it’s caught early. I want our patients to know there’s more to them than being a smoker, and that we’re not here to shame them.”
That’s why Giordano dedicated her award to her father, and why she continues to serve patients with compassion – although she is reluctant to stand in the spotlight.
“When I talk to patients and welcome them, I try to put them at ease and love on them. I want to be that nurse who is smart and gentle, who makes you feel like family but also that we’re going to take care of you,” she said. “Being an outreach coordinator is something I get to do.”
Randy Mintz, a registered nurse with the ECU Health Enterprise Resource Team, began his nursing career in 1999, and he joined ECU Health in 2009, but health care was not his first career.
“I was in the military,” he said. “My dad and brother were in the Air Force. My dad was from Wilmington, and I grew up there until I was 14 or so and we moved to Wichita Falls, Texas. When I finished high school, I wasn’t sure what I wanted to do, but I didn’t want to stay there. I decided to give the military a shot.”
After his four years in the Air Force, during which time he was stationed in Germany and then New Mexico, Randy signed up for the National Guard, where he served as a medic.
“I think working in health care was always in the back of my mind,” Randy said. “In the Air Force I considered an EMT class, but it just didn’t work out and I let it go.”
Once he was out of the military, Randy wanted a stable career with benefits, and he decided to enter law enforcement. He found a job in a detention center, but a few weeks in, he met Pat Kosman.
“We had a few inmates who were sick, and Pat was a gruff, older nurse who worked there. She said, ‘Randy, you should go to nursing school.’ I told her she was crazy – I was going to be a cop.”
At the same time, Randy was in school where he took sociology, psychology and criminal justice classes.
“The college was kicking off this EMT program, and one of the instructors asked if I wanted to take an EMT basic class. I thought it was a good idea because in law enforcement, as a first responder, it could be a good opportunity.”
Randy took the class, and then he took the intermediate class.
“It was kind of fun and I did really well. And in the second class, I had awesome clinicals at the hospital.”
And who was his preceptor at that hospital? Pat Kosman.
“When the clinicals ended, she told me I really needed to go to nursing school. She said, ‘you’ve got a knack for this.’”
Randy “flipped the switch” and spoke with his advisor about changing his career plan to nursing. She helped him fill out the application for nursing school, and a few weeks later, he was called in for an interview with the program director.
“There were a few pre-requisites I needed to complete, which would take another semester, and I got in. I was like, wow – I’m really meant to be here. That’s how it all started.”
“And Pat – she was instrumental in making it happen. I’m not sure what she saw in me, but she set the path in motion,” Randy added.
Randy said his work in the military has shaped the way he approaches nursing, specifically how he interacts with his colleagues and leadership.

“When you’ve been a nurse for 26 years, you lead different teams and you want to treat everybody you work with the way you’d want to be treated,” he said. “Especially if you’re in a leadership position – you want your team to know you work for them. You’re there to serve them and make their world a little bit better.”
That carries over to his current role with the Enterprise Resource Team.
“The team is like the central staffing office for the entire health system,” he explained. “I go to the Medical Center, Edgecombe and Beaufort, but the system is set up by region, and you pick which region you’re in. Then you get an email or text at five in the morning that tells you where you’re going that day, where you’re needed.”
While working in a variety of locations can be challenging, Randy said it provides insight into how different departments function.
“You bring some good influence and values, and it offers a different way of thinking and doing things,” he said.
To anyone considering a career in health care, Randy said he had some advice for them.
“Health care, and nursing especially, is a great opportunity to provide for yourself and your family. The investment up front may seem like a lot, but there are so many opportunities, from clinical education, leadership, nurse practitioner, CRNA – you may not even realize how many there are until you’re in it. The beginning is the same, but there are different pathways you can take.”
Randy’s path hasn’t been a straight one, but he doesn’t regret his decision.
“I never thought I’d be doing this, but it’s been really fun,” he shared. “I’m happy I was pushed in this direction. We have the opportunity to take care of our community, and whether you’re in one of the community hospitals or the Medical Center, you’re making a big impact.”
At 80 years old, Berry Warren, a medical lab technician, has seen his fair share during his 45 years at ECU Health.
“I was working for a wholesale company but felt like I wasn’t really helping anyone in that role,” Warren said. “Then my sister-in-law and brother-in-law suggested I go to nursing school. Nursing wasn’t really for me, but I enrolled in a Medical Laboratory Technician program near Asheville and was hired to work in the lab of the local hospital before I graduated.”
After working in and near Asheville for several years, Warren joined ECU Health in 1981. Over the years, he’s worked at ECU Health Beaufort Hospital, ECU Health Chowan Hospital, ECU Health Bertie Hospital and ECU Health Medical Center.
“At smaller hospitals, you get to know the patients and talk to them,” he shared. “You also get to do a little bit of everything. But at the medical center, you learn a lot because you see more diagnoses and patients.”

His wife and his daughter have also worked at ECU Health, making it a family affair.
“I’ve been in health care for 55 years,” he said. “And between me and my wife and daughter, we probably have close to 80 years of time with ECU Health.”
Working in the lab, Warren said he has served in many roles, but one he especially enjoyed was working in the cardiac surgery unit.
“In 1984, they sent us to Duke to work in the operating room while they were doing cardiac surgery,” he explained. “Dr. [W. Randolph] Chitwood was one of the surgeons and he always took time to talk to me, even though I was a lowly lab technician. And he taught me things – like he’d show me the heart during surgery and describe the parts and how they worked.”
Warren explained that during surgery, it was his responsibility to calculate blood gases and clotting time for patients.
“You have to thin the blood to work on the heart,” he said. “And we use heparin to do that. We had to determine a baseline clotting time using an actual graph on paper, and we’d calculate how much heparin the patient needed to thin the blood to go on the heart and lung machine. Then we had to calculate how much Protamine sulfate, which counteracts heparin, to give the patient after the surgery so their blood wouldn’t be too thin in recovery.”
Now, Warren said, much of that manual work is done by computers.
“I didn’t grow up with computers, but everything is computerized now,” he said. “I used to do blood cell counts manually using a microscope, but things have changed so much and so fast. The team I work with helps me out when I need it. We’re all buddies.”
Warren was recently recognized at the ECU Health Appreciation of Excellence Gala with a plaque commemorating his 45 years of service. And while he doesn’t have a specific date in mind, Warren said he will eventually retire. When that day comes, he doesn’t plan to sit around.
“My wife and I live on a farm so there is always wood to cut or a yard to mow,” he said. “I also mow my church’s grass. I don’t want to sit around the house; I like to get out and spend time with my wife.”
To new team members joining ECU Health, Warren said it’s worthwhile to keep up with changing technology.
“Don’t let it overpower you,” he said. “Jobs evolve and you have to change with it. Always be learning.”
To be a health care provider is to answer a calling. For some, the journey to health care is a straight line; for others, the road is winding. This series features stories from ECU Health team members who took the winding road, but found the destination to be worth the effort.
Tim Barnes, the clinical manager for radiation oncology, has spent 17 years with ECU Health, but a career in health care wasn’t his original plan.
“I grew up wanting to work in law enforcement,” Barnes said. “My four-year degree is in criminal justice and in 1996, I started my career at the Wilson Police Department. I worked there until 2006 and served in various roles from patrol officer to the SWAT team to homicide.”
Somewhere along the way, however, Tim felt called to do something different.
“Medicine and law enforcement are both fields you have to feel led to do,” he said. “As a child and through high school and college, I had a strong desire to be in law enforcement. But somewhere along the line, and maybe it was because I was getting older or was married and had a family, there was a point I felt a calling to the medical field.”
Having a close friend diagnosed with head and neck cancer planted the seed for working in health care.
“When my friend passed away, that directed my focus on cancer care specifically. So, I started researching different jobs and opportunities where I could transition from law enforcement into the medical field,” Barnes said.
That’s how Barnes ended up in radiation therapy.
“I drove over to Pitt Community College and looked into their Radiation Therapy Technology program and met the program director at the time, Elaine Spencer,” she said. “She explained the process of going back to school and I just followed her advice – which is how I ended up here.”
Barnes joined ECU Health in 2009 as a radiation therapist, when radiation oncology was a part of the Brody School of Medicine.
“I worked there until the radiation oncology department moved into the new cancer tower, and I’ve been there ever since,” he said.
Barnes said that although law enforcement and medicine don’t seem connected, there’s a lot he applies from his experience as a police officer to his current role.
“It’s obviously a very different job, but my attention to detail, my focus on safety and the importance of working as a team – I learned those skills from my time with the police,” he said. “It’s very high risk in law enforcement, and you learn to depend on each other and function as a team. That carries over into the medical field and how departments and teams coordinate to take care of patients.”
That collaboration and support is very important to Barnes.

“I have always felt like I belong here,” he said. “We have an awesome team. To do what we do, you must feel led here, and the people on my team are here because they care. It’s not just a job; our people are doing more than just a technical service. They believe in what we do and really want to care for our patients.”
That’s only one reason why Barnes said he would gladly advise anyone to pursue a career in health care.
“There are so many options and opportunities, so you can go out and research to see what fits your lifestyle and interests,” he said. “I chose radiation therapy, but that’s just one specialized area. There are those who treat patients directly, but there are other options, too. Nothing works if you don’t have leadership and administrative support. Nothing stays clean without the environmental support staff. If someone isn’t sure what’s right for them, I’d highly suggest they look into health care.”
Barnes said a lot of people are surprised when they hear he was a police officer, but for him, the transition to health care makes sense.
“People hear I worked in homicide and say that’s such a big jump to treating patients,” he said. “It is definitely different, but I’m still doing a job where I serve and help people, and really, that’s what matters at the end of the day.”
Dannica Ashnault, an orthopedic surgery physician assistant (PA), joined ECU Health in December 2025, and so far, she’s loving her new role.
“The team I work with is great,” she said. “Everyone has been so nice and welcoming, and it feels like a family.”
Dannica isn’t just an exceptional provider, however. She’s also a former Olympic-trained skier who started competing early.
Dannica grew up in New York state, began skiing at one and a half years old, and at age 14, she moved from home to attend high school at the Burke Mountain Academy in Vermont, the nation’s first elite ski academy.
“I had to decide at 14 if I wanted to go all-in on skiing, and looking back on that now, it seems crazy. I was living in a dorm, doing my own laundry and managing my time with school and skiing. It was a different way to grow up,” she said.

Her parents drove up every weekend to visit and watch her ski, and during the week, Dannica and her classmates adhered to a very strict regimen.
“I’d wake up, work out, eat breakfast, take classes, have lunch, have more classes, work out again, and if it wasn’t the winter, meet with the coach and watch videos,” she shared. “In the winter, I’d wake up, ski and train until lunch, have class after lunch, workout, tune skis, eat dinner and watch video. Then I’d go to bed and start over the next day.”
Such a structured life yielded great outcomes for Dannica and her classmates when it came to skiing, but by the time her senior year rolled around, she had a decision to make: continue skiing and training in the hopes to make the Olympics, or go straight to college. She chose the latter.
“I never went to a football game in high school. I never attended prom,” she said. “I wanted to be normal, to start my life. I love skiing, but I wanted other things too.”
One of those things included pursuing a career in medicine – something she’d been thinking about since sustaining an injury during a race.
“At 15, I had a really bad crash and blew out my knee in multiple places,” she said. “I was also knocked unconscious for eight minutes, so I had a pretty bad concussion.”
The injury meant she couldn’t ski, but it also meant she spent a great deal of time with her sports medicine team.
“I couldn’t have surgery until I could squat a certain weight, because they wanted me to get back to skiing as quickly as possible,” she recalled. “My surgery was five or six weeks after the injury, and when I woke up in my room, the surgeon was in my room with my parents, telling me to get up. I had a whole team around me and supporting me so I could get back to what I loved to do. I wanted to be a part of that experience for someone else, and that got me interested in medicine.”
After high school, Dannica attended Boston College, where she continued to ski for its Division I team.
By her junior year, however, Dannica said she was burned out. She wanted to start her life and career, and although she’d been considering medical school, she pivoted to PA school because of the flexibility it offered her.
Now, Dannica skis for fun, and she enjoys watching her former classmates find success in the sport.
“I’ve been waking up to watch the Olympics,” she said. “The ski racing community is so small, and it’s cool to see what they’re doing. My former lifting buddy in high school, Nina O’Brien, competed in the Olympics, and my classmate, Mikaela Shiffrin, just won gold in slalom.”
Dannica said she enjoyed her time as a competitive skier, but being a part of a team that sees patients through their care journey is just as rewarding.
“I wouldn’t trade my experience as a skier for the world, but I love what I do,” she said.
It was a quiet day in the cardiology clinic when the echocardiogram technician at ECU Health Beaufort Hospital asked Michael Joyner, a nurse practitioner, for a favor.
“My schedule wasn’t full because I had only been working at that location for about a month, and the echocardiogram tech had a student,” Joyner said. “Their patient didn’t show up, so she asked if her student could practice using the equipment on me.”
When the student viewed Joyner’s heart, however, something unexpected showed up.
“I knew I had a heart murmur, but the technician looked concerned and took over the scan. Turns out my aortic root was dilated to more than twice its normal size,” he said.

The aortic root is where the aorta, the largest blood vessel in the body, is closest to the heart. A dilation, otherwise known as an aneurysm, is potentially life threatening.
“When you research aortic aneurysms, one of the first things you read is that the first symptom is often sudden death,” Joyner said. “They’re often asymptomatic, but if it ruptures, usually the only thing people can do for you is hold a funeral service.”
Help was only a call away
After the scan, Joyner spoke with a cardiologist immediately. It helped that he knew trusted team members from across the system.
“I asked one of my former students and a nurse practitioner, Brooke Kostok, if her colleague, Dr. Ben Degner, could look at my echocardiogram,” Joyner said. “He called me personally that afternoon and spent 20 minutes on the phone outlining what he thought about it and his recommended next steps. He didn’t have to do that.”
After a computerized tomography (CT) scan and an official diagnosis, which showed the amount of dilation was borderline, Michael and his physicians opted for a watch and wait approach.
“I had a new grandson on the way, and I didn’t want to be recovering from surgery during that time,” he said.
A repeat echocardiogram in the fall of 2025 showed the dilation had grown by a small amount. Joyner decided it was time to have surgery, and on Oct. 21, he underwent an aortic root replacement with aortic valve replacement and reimplantation of the coronary arteries – also known as the Bentall procedure.
“It was a long surgery, and I was lucky to have a network of people I could rely on for support, including Chris Baxter, a certified registered nurse anesthetist (CRNA), who was with me during the surgery,” Joyner said. “I wanted him at the head of the bed during my surgery because I had full confidence in him.”
Other colleagues provided support during the surgery by placing a PICC line or being present and supportive for Joyner’s wife, Gwin, and their son.
Recovery went well until day three, when Joyner experienced some post-operative atrial fibrillation – a not uncommon event after this type of surgery. Another former student, D.J. Smith, ACNP on the CVICU, helped restore Michael’s normal heart rhythm.
After seven days in the hospital, Joyner went home, but six weeks later, a post-operative CT scan showed some leakage at the site where an intraoperative cannula had been placed. He needed another surgery in December 2025.
Looking forward to the future
Taking nearly four months off work and undergoing two surgeries has been tough, but now Joyner is feeling better every day.
“It’s difficult to reconcile that you need surgery when you feel healthy. And when you work in health care, you know what could go wrong,” he said. “To have two surgeries – to have your chest opened twice – that’s a difficult recovery.”
Despite the mental and physical challenges, Joyner is clear about his perspective of gratitude.
“I don’t believe in coincidence,” he said. “So many things had to happen to get me where I am. I had to find out about the job at Beaufort – because I wasn’t looking for a new role – and then get the job. I had to be in the clinic that day and not have a patient. The echocardiogram tech had to have a student and a patient cancellation. It was a series of events coordinated by God.”
Joyner is scheduled to return to work in March, and he’s thankful to all the people who played a role in his diagnosis and recovery – especially his wife.
“Gwin is also a nurse at the hospital, but during this time she was my personal nurse and physical therapist,” Joyner said. “I’m fortunate to work in a profession where I was in the right spot at the right time, and to have a whole network of people I can call. That’s made the difference for me.”
Washington, NC – ECU Health Beaufort Hospital is proud to recognize Leslie Alston, RCP, RRT, as the 2025 Pulmonary Health and Illness of the Lung (PHIL) Award recipient for ECU Health regional hospitals. The PHIL Award, established by the FACES Foundation in honor of Philip C. Lamka who passed away from Interstitial Lung Disease (ILD), honors respiratory therapists who demonstrate exceptional compassion and patient-centered care.
“Leslie represents everything the PHIL Award stands for,” said Dr. Dennis Campbell II, DHA, RN, FACHE, president of ECU Health Beaufort Hospital. “Her compassion and professionalism make a lasting difference for patients, families and our care teams. Leslie is widely respected by patients, families and colleagues for her clinical expertise, calm leadership and ability to provide comfort and guidance during life’s most critical moments.”

Alston, who has been a respiratory therapist for 28 years – 20 of those spent at ECU Health Beaufort Hospital – is equally respected by nursing leadership and educators. New graduate nurses and code teams rely on her expertise during training and emergency situations. Known as a natural coach, she provides guidance in a supportive and encouraging way while maintaining a strong focus on patient care. She also assists with nursing and CNA skills fairs and represents respiratory therapy at local middle and high schools, emphasizing safe, high-quality, person-centered care.
“I am truly humbled by this recognition, but the greatest reward comes from caring for my patients. Every day, they remind me why I am passionate about being a respiratory therapist. It is an honor and a privilege to support them, and their gratitude and trust are the motivation that keeps me dedicated to this profession,” said Alston
Alston’s impact is reflected in the many calls and handwritten notes from patients and families following discharge. These messages consistently highlight Alston’s personalized care and the genuine concern she shows for each patient. Families often share how Alston took time to listen, explain and provide comfort during some of the most difficult moments of their lives.
Physicians throughout the hospital also recognize her excellence and frequently request her by name to care for their patients. Medical and physician assistant students regularly shadow her to gain a better understanding of respiratory therapy.
FACES Foundation recognizes two PHIL Award recipients each year — one from ECU Health Medical Center and one representing ECU Health regional hospitals. Alston was named the regional recipient.
Chris Mintz, an RN with ECU Health’s Enterprise Resource Team (ERT), has always felt drawn to community health rather than inpatient bedside care.
“I’ve worked in a pediatric clinic, same-day surgery, home health and hospice care, and inpatient and outpatient case management,” Chris said. “I was a supervisor and manager in case management and hospice care, and then director of nursing for mental health and substance abuse treatment.”
When the priorities for integrated health care shifted, she needed a new path.
“I decided I wasn’t too old to learn something new, so I joined the Beaufort Hospital emergency department (ED) to work at the bedside,” she said. “The rest is history.”
That serendipitous job change led Chris to meet Randy Mintz, her now husband and fellow nurse.
“Much of the work in the ED is community health,” Chris said. “The ED is full of people without access to care. It is all some people have, and we take care of them the best way we can.”
Meant to be
Randy was working night shift in the ED when he received a call.

“The manager asked me if I could precept someone new to the ED who needed extra help,” he recalled. “Funny enough, I really didn’t want to do it.”
“Originally, I was assigned to another seasoned nurse as a preceptor,” Chris added. “But she didn’t feel like she wanted to do it at the time, so they asked Randy for a favor. Now we thank that nurse all the time for putting us together.”
Randy took the time Chris needed to help her learn the ropes.
“It meant a lot to me. I was nervous and wanted to be sure I had the skills I needed to take care of our patients,” Chris said.
From there, Chris and Randy said they discovered they shared a higher level of compatibility.
“We laughed at the same jokes, and she got my dark sense of humor,” Randy said.
But even better, they found they made each other better nurses.
“I had worked in the ED for a while and was a little hardened. She was like a marshmallow. She oriented me on how to interact with people and to look at things differently. As much as I taught her about the ED, she taught me how to be better with people,” Randy said.

“I am 100% positive that had she not come to the ED, and if that other nurse had agreed to be her preceptor, all the good things that have come my way would not have happened. It’s all her doing.”
“The only way I have been able to work at this level is because of him,” Chris said.
Love takes flight
“Four years went by like a flash, and we got engaged. But I was hesitant about getting remarried,” Chris shared. “One day, I saw there was a hot air balloon festival in Statesville, and I said to Randy, ‘You want to get married in a hot air balloon?’ He said, ‘absolutely!’ and that’s what we did.”
Randy and Chris married at sunrise on Oct. 19, 2025.
“We found a company that marries people all over the world, with real officiants. We had a small, very personalized ceremony right there in the balloon. Then we got to enjoy the rest of the festival and our wedding funnel cake,” Chris said.
Now they get to work together on the same team.
“After my interim assistant nurse manager role in the ED at Beaufort, I heard about the Enterprise Resource Team, and it was an easy transition,” Randy said. Chris joined shortly thereafter.
The Enterprise Resource Team meets staffing needs at ECU Health Medical Center and ECU Health Community Hospitals based on census and staffing.


“The Resource Management team assesses needs based on feedback from the medical center and our community hospitals, where they find out about staffing deficits and prioritize who needs what. That’s not an easy job,” Chris said.
“You can choose the region and specific department or specialty you want to serve,” Randy added. “Then you get a text at 5 a.m. or 5 p.m. to tell you where you need to go.”
Randy and Chris said it is nice to be able to work in the area they chose, but at different locations where they are needed.
“Our goal is to lighten the load for the staff where we are assigned and to take great care of their patients,” Chris said.
It’s an added bonus to work together.
“There are some days we might be able to grab a coffee together or only say hello as we’re walking by, but we always know the other one is there,” Randy said. “Other days, we’re working side by side, and those days are the best. You have a person you know and trust, and you know their strengths, and they know yours. It makes it nice.”


