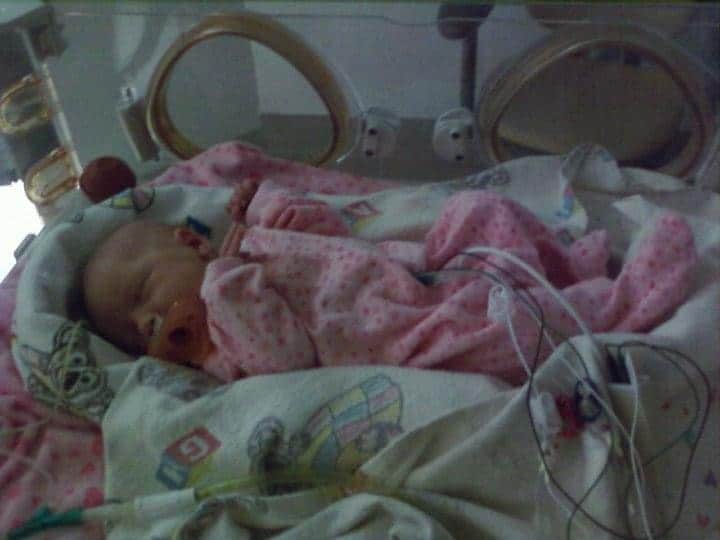
Jamysen Howard during her NICU stay in 2010.
From premature babies to complex conditions, the Neonatal Intensive Care Unit (NICU) at James and Connie Maynard Children’s Hospital sees the youngest patients at ECU Health Medical Center and provides high-quality, compassionate care while looking after families throughout their NICU journey.
Along the way, many families find a community and support system around them as they navigate the experience.
Thriving 12 years later
Tonya Howard found out at her 11-week ultrasound that her daughter would be born with her intestines outside of her body, a condition called gastroschisis.
While baby Jamysen grew, plans were lining up to have a pediatric surgeon join the team at Maynard Children’s Hospital at ECU Health Medical Center just in time for Jamysen’s arrival. However, when she came four weeks early, the pediatric surgeon received emergency privileges and successfully operated on her just after her birth.
Tonya said the supportive care team helped her and her family immensely during their time in the NICU. While they took care of Jamysen, they also kept the family up-to-date and informed.
“The NICU nurses who, probably about four or five of them I still talk to, kept me up with Jamysen’s progress,” Tonya said. “I had two other children at home, so I’d go home and spend the night and when I’d get up in the morning, the first thing I’d do is call the NICU to see how she did that night. The nurses were the ones that took care of her and they were with her all night.”

Jamysen is now in 7th grade, excels in school and plays volleyball for her school and travel teams.
She also said the NICU community is very strong and has been happy to serve as a support to other NICU families, including one that experienced gastroschisis, just like Jamysen.
Today, Jamysen is 12 years old and thriving. Tonya said while they were told there was possibility Jamysen could experience trouble with physical and mental development, she is now an honor roll student and plays volleyball with school and travel teams.
“We’ve always told her that she can do anything she wanted to do,” Tonya said. “I was like, ‘before you were one day old, you’d already been through a five-hour surgery so you know what, you can do anything you want to do.’ And she’s done just that. She knows she’s tough, she’s never had much fear and she’s headfirst into everything and always has been.”
Jamysen frequently participates in Children’s Miracle Network events as well.
Tonya has a unique perspective on the Maynard Children’s Hospital as a former team member in the pediatrics department, including time before the Children’s Hospital was built.
“At one point the NICU was just one big room. When Jamysen was born, the NICU was what it is now and each baby had their own individual room,” Tonya said. “Everything from the beds to the Child Life [team] and now they’ve progressed to where the parents can even log on and see their babies when they’re not able to be there. We didn’t have that while we were there but that’s just amazing.”
Rallying around Waylon
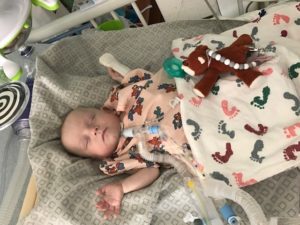
Waylon Denny is shown in a crib after having a tracheostomy.
On July 23, 2016, Waylon Denny was born at 23 weeks, weighing 1 pound, 4 ounces. He spent the first 298 days of his life at the Maynard Children’s Hospital, beginning with about four months in the NICU.
Following a surgery for young Waylon, he became sick and needed immediate intervention. His providers knew one treatment, called extracorporeal membrane oxygenation (ECMO), could be lifesaving.
“I mean, they all really rallied right around us,” Waylon’s mother, Sara, said. “They got the doctors and everybody in the PICU that had anything to do with ECMO to come down to look at him to see if he would be a candidate for ECMO. And I truly believe if it was not for his respiratory therapists and nurses fighting for him that day I really do not believe that he would even be here.”
ECMO is a treatment where blood is pumped out of your body and into a machine that removes carbon dioxide and then flows blood back to tissues in the body. One of the providers fighting for Waylon was Dr. Shannon Longshore.
“I remember Dr. Longshore telling us that in a baby his size, 23 weeks, he was already swollen,” Sara said. “Everything he had been through, she should not have been able to get the [tubes] in his neck. And I remember her telling us that she looked at the team in that room and told them that she was going to keep trying because we were two weeks away from going home. And she closed her eyes and told God if it was his will or for him to live, they would go in. Well, those [tubes] went in.”

Waylon started kindergarten this year.
Sara was a first time mom and said it was hard to know what questions to even ask. Luckily, she said, the doctors, nurses and respiratory therapists were there to help. They explained things to her and the family and checked on them frequently.
Six years later, the check-ins have not stopped, she said.
“We’ve had so many nurses, doctors, respiratory therapists, physical therapists and occupational therapists friend us on Facebook just so they can keep following him and see how he’s doing,” Sara said. “And then when we were able to go to the hospital before COVID, and we would go and visit the NICU and the PICU and everywhere where he had been.”
Waylon is six and starting kindergarten and has met every challenge he’s faced in his young life head-on.
September is NICU Awareness Month and Sara said that she and Waylon have NICU Awareness Day (Sept. 30) t-shirts that they wear each year and she’s looking forward to celebrating and recognizing the day once again with her miracle son.
Twins fight through NICU together
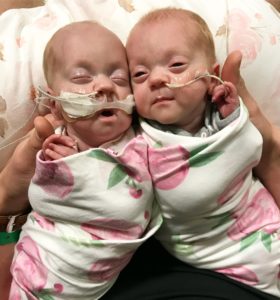
Twins Molly and Lucy Davis are shown during their NICU stay.
Owen and her husband Garrett Davis were expecting twins and enjoying a family vacation before welcoming the new additions to their family. But their vacation was cut short when Owen could feel something was not right and she went into labor at 22 weeks.
Molly and Lucy Davis came into the world each weighing just 1 pound, 9 ounces and were immediately placed in the NICU at Maynard Children’s Hospital. The twins were both fighting infections early on in their lives and experienced many tests, treatments, procedures and exams over their 128 days in the NICU.
Owen said they experienced the full range of the NICU rollercoaster during their stay, but they were comforted along the way by the supportive and caring team at the hospital.
“One of the biggest things that I remember were the nurses and our neonatologists,” Owen said. “We still keep in touch with them really on a daily basis. Some of our nurses babysit for us, which is really special. Just the people that we encountered throughout our long stay made it bearable.”
Along with the great support of care teams, Owen said some of her family’s closest friends came from their time in the NICU. She said it is a special bond and shared experience for families of NICU children.
Recently, Owen had someone reach out to her on social media saying their friend was about to have a child at 23 weeks and the two got in touch with each other.

The Davis family takes a photo at the beach.
“It’s really cool to have that connection and to be able to provide insight and support to other families going through what we’ve been through,” Owen said. “So I’ve been in touch with basically a stranger from across the country who saw our story and reached out for some guidance and just a listening ear to be able to bounce questions off of and support and vent. It’s hard to understand unless you’ve been through it.”
Being open with her family’s story has brought comfort to others and she’s happy that her twin daughters are beginning to understand their own story as well.
She said it’s important to her that Molly and Lucy know how strong they are and that their parents advocated and fought for them from the time they were born.
“It was super hard and trying, but it’s also their testimony and they understand that at 3 years old. It’s really two miracles that we were able to witness,” Owen said. “They know, as much as a 3-year-old can. We have their blessing beads, these little beads that they got for every procedure and every test they had, we have them hanging up on their beds and we have their first diapers that are about the size of a credit card. We keep two of those on our entryway table in our living room as a constant reminder of what they’ve been through.”
Owen said she has a video that she put together of her daughters’ NICU stay that shows up in her memories each September and serves as a reminder of the importance of the month for her family — and so many others.
Resources
Meet Clive, ECU Health Medical Center‘s resident canine.
“Currently, he’s working two days a week with us,” said recreational therapist and dog handler Kasey Shue. “Some mornings when we go through the hospital doors, he’s just like, on a mission. I have to be like, ‘Clive, wait, hold on, buddy. You’re like, ready to roll this morning’. So I think he knows what he’s here to do.”
It’s an assignment he’s well prepared to tackle.
“A service dog is specifically trained to do certain tasks for somebody with a disability,” said Clive’s owner and outpatient rehab supervisor Tanya Bowen. “So a therapy dog is basically to provide comfort and they have to be very friendly and outgoing because there’s a lot of people that want to pet them and touch them. They have to be calm. They have to like the interaction, the social interaction. So he’s kind of like a little combination of both.”
Clive’s skill set benefits patients in a number of ways, whether that’s assisting with physical needs or providing emotional support.
“We’ll partner up with a physical therapist or an occupational therapist and we’ll work on walking him if they’re working on mobility improvement,” Shue said. “We’ll work on throwing a ball if they need some hand strengthener. We’ll work on them being able to pick up a very small treat and hand it to him if they have fine motor limitations. We really try to incorporate him into whatever functional skills they are trying to learn to make their life easier when they get home. On the other side, many times we have patients that are depressed or anxious. They don’t like being in the hospital and he just provides that comfort.”
And his services are in demand at the bedside and beyond.
“He actually wears a vest that says, I’m friendly, please ask to pet me,” Shue said. “We absolutely encourage that because he is therapy for our patients, but he’s also therapy for the staff, the families.”
Resources
ECU Health Therapy & Rehabilitation
Watch more ECU Health News videos
At ECU Health, team members go above and beyond to form trusting relationships with patients and their families to better serve eastern North Carolina.
Over the last 14 years, Occupational Therapy Assistant Winnie Miller worked one on one nearly every week with Taylor Anthony, who is now preparing for his freshman year at the University of North Carolina Wilmington. Taylor is autistic and began receiving treatment from an occupational therapist when he was 3 years old.
First steps
Kim Anthony, Taylor’s mother, recalled the early days of her son working with an occupational therapist.

“He was my first child and had special needs,” Kim said. “I remember walking in and just being terrified – you don’t know what your future looks like, or his future, or will college even be an option.”
After about a year of working with a couple of other occupational therapists within the health system, Miller stepped in and began her treatment sessions with Taylor.
Miller said their work together started with the base steps – figuring out hand dominance, holding pencils, learning to write, forming letters and coloring within lines.
Kim said as Taylor reached school age, she’d be frustrated when hearing about things that people believed Taylor could not do. But she knew she could turn to Miller and her expertise to come up with a plan to help Taylor reach his goals.
“I would email her and be like, ‘I’m struggling with this’ and she would be like, ‘OK we’ll figure it out,’” Kim said. “She would have checklists for him and just everything. It was amazing. She was the biggest support system I had.”
Hitting their stride

As Taylor got a bit older they worked on how to tie shoes and other fine motor skills. Then it was on to processing your environment and communicating clearly, social aspects of life, how to drive, and other elements of college life and living independently.
Miller compared her role as an occupational therapist to being a coach, with the patient’s supportive family as the team.
“The coach can give suggestions and a play-by-play plan of what you need to work on, but we’re just a little snippet,” Miller said. “I’m only with him an hour a week. They, as a team, have to work on those skills 24/7. I knew they were doing their work at home and there was always going to be follow through.”
Taylor’s father Stephen Anthony, director of service line development for Women’s and Children at ECU Health, said Miller’s out-of-the-box thinking greatly benefited Taylor’s growth into the young man he is today.
Miller broke down the learning process, kept his steps very goal-oriented and stayed in frequent contact with the Anthony family along the way.
“She made it manageable; she made it like they were just going to visit with each other. It wasn’t like a clinical visit, it was just, ‘Hey let’s go in my office and look at some stuff,’” Stephen said. “Maybe they do some stuff on the computer, maybe they use the kitchen to make some eggs or something like that, safety skills with the oven. Stuff that nobody would ever even think of.”
Off and running
These visits also included working with Helen Houston, an occupational therapy driver rehabilitation specialist, who addressed Taylor’s fitness to drive, to ensure he could approach driving safely.
Stephen said Taylor took one test as he was approaching driving age that showed his reactions and reflexes were borderline to be a driver. Before he took a driving test, he was put through the same tests, which showed about 75 percent improvement thanks to his hard work. Now, Stephen said Taylor is just as good a driver as anyone and probably safer than most his age because of the work he’s done.
Taylor said he was thankful for his time with Miller and he’s excited to take all he’s learned to Wilmington.
“It has meant a lot,” Taylor said. “I’ve definitely learned many things. It also took a lot to learn from a different perspective. My family means a lot. They’ve done everything for me to be sure I’ll be the most prepared human being. They’ll know I’ve learned enough to make good decisions and they’ll be supportive of me no matter what.”
As Taylor prepares for his first year of college, one where he’ll also compete as a member of the UNC Wilmington Cross Country team, his family knows he is prepared for different aspects of college life, thanks in part to his work with Miller.
Miller said she loved working with Taylor and can’t wait to visit with him when he returns from school and hear about his college experience.
“He was always an hour a week that I looked forward to,” Miller said. “He always had a new question for me or something new that kept me on my toes and I didn’t know what was going to be the question of the day, what we were going to have to explore and figure out. I really enjoyed that challenge. I’ve loved every minute.”
Resources
Learn more about Therapy & Rehabilitation services at ECU Health.

For the Eastern Carolina Healthcare Preparedness Coalition (EHCPC), being ready is part of the job.
“What we have here is our field communications support truck,” said Matt McMahon, disaster services specialist with EHCPC. “This is essentially the heartbeat of our mobile field hospital.”
From trucks that double as mobile hospitals to coordinating evacuations or the deployment of medical supplies, the coalition remains on standby for when emergencies strike or networks go down.
“So, if a hospital loses communication, whether it be phone, radio or internet, we can come and support them,” McMahon said.
The coalition provides a critical line of support, whenever and wherever it’s needed most. As they prepare for hurricane season, they want you to do the same.
“We want people to be prepared, and starting a hurricane kit is the first step in doing so,” said Chris Starbuck, health care preparedness coordinator for EHCPC.
A basic kit includes important items, like water, food and other supplies to last several days. Ready.gov is a federal government website with helpful information about how to properly prepare for a hurricane. Creating a plan that meets the specific needs of your household and building an emergency kit that contains at least 72 hours’ worth of supplies can help you stay adequately prepared for a natural disaster like a hurricane.
“Put all your important documents together – marriage certificates, birth certificates, wills,” Starbuck said.
Another item for your hurricane prep checklist – help others plan, too.
“Work with your neighbors, your communities, churches, because if we can prepare them, we can make a more resilient community overall,” Starbuck said.
Resources
Hurricanes can form quickly. Take the time now, before a hurricane impacts our region, to educate yourself on how to prepare and respond. Below are helpful links for federal and state websites:
- Ready.gov – Hurricane Information
- Ready.gov – Make a Plan
- Ready.gov – Build a Kit
- ReadyNC.org
- ReadyNC.org – Emergency Alerts
- ReadyNC.org – Evacuation Routes
- ReadyNC.org – Know Your Zone
Watch more ECU Health News videos

Dr. Michael Waldrum
When the new ECU Health brand was announced earlier this year, it was launched with a singular vision: to solve complex health care challenges preventing eastern North Carolina from realizing its immense potential. We know that a strong and vibrant health care system is necessary to grow and sustain healthy communities. Our region, which is home to 1.4 million hard-working people, faces disproportionate rates of chronic conditions – conditions that, when not managed early, result in high medical bills and financial hardship, particularly for those without insurance.
I am proud of the work we’ve done here in the East to create a premier academic health care system and none of this is possible without the incredible work by our health care professionals. They are living the ECU Health mission each and every day by purposefully delivering health care in our communities and training the next generation of health care professionals.
While we have much to be grateful for, it is also necessary to recognize the current state of health care across the nation, within all of North Carolina and here at home. Health systems and hospitals are facing financial challenges largely driven by the pandemic, labor shortages, inflation and market disruptions. Despite careful planning and the tireless efforts of our team members, ECU Health is facing the same unprecedented challenges as other health systems. Some of our current challenges stem from unexpected and extremely high labor costs in addition to the rising cost of supplies like medicine and equipment, which are significantly higher than they were just one year ago.
In rural regions like ours, navigating these realities is even more difficult. We already face a high burden of disease, a large geographical area where local providers and teams provide a literal lifeline to quality care and a large number of community members who don’t have access to adequate health insurance.
While we are making great progress in charting the future of health care in the East, the reality is our rural communities need immediate support from our elected officials on two fronts:
Medicaid Expansion: for years, ECU Health has consistently and vocally advocated for expanding Medicaid to support rural communities in North Carolina. Expanding Medicaid would increase access to high quality care for more than 500,000 North Carolina residents and provide coverage to treat chronic conditions, prevent illness and disease progression and support healthy, productive lives. It is the right thing to do for all of North Carolina and especially in rural communities where access to care is always a challenge.
Healthcare Access Stabilization Plan: health care across the state is also relying on state lawmakers to support this federal program that would provide North Carolina hospitals with up to $1.8 billion in funding. At no cost to the state, North Carolina can apply for this level of funding as a result of moving to Medicaid managed care. This program can help stabilize the financial well-being of rural hospitals as they continue to recover from the chaos of a worldwide pandemic.
As someone who has dedicated their career to health care, I know that in order to meet eastern North Carolina’s full potential, we must embrace the fact that a healthier community is a more economically vibrant community. It is imperative that we do not lose this opportunity to implement programs that will have life-changing impacts on so many North Carolinians. That is why it is vital that the General Assembly pass Medicaid expansion and move forward with HASP funding. Together, these efforts will help close the insurance gap, provide care for our most vulnerable community members, lower medical bills, bring much-needed dollars to the state and allow health systems and hospitals to continue to provide high-quality care to those who depend on it.
Michael Waldrum, MD, Chief Executive Officer, ECU Health
While skin cancer is less common in African Americans, experts say death rates from melanoma are much higher in the African American community. Melanoma, which often presents as an irregular mole, can spread much quicker and easier than most other skin cancers and can produce worse outcomes. Melanoma is often found in later stages in African Americans when treatment can require more intensive surgery or even radiation or chemotherapy. Knowing the signs and symptoms can help catch melanoma early, when the cancer can be cured.
African Americans are up to four times more likely to be diagnosed with advanced melanoma and 1.5 times more likely to die from melanoma, according to the Melanoma Research Alliance. This is alarming, considering African Americans account for a small portion of melanoma diagnoses.
Skin cancer is the most common type of cancer. The three major types of skin cancer are basal cell carcinoma, squamous cell carcinoma and melanoma. Basal cell carcinoma and squamous cell carcinoma can present as pink or scaly lesions that are not healing or spots that are bleeding, itchy or painful. These forms of cancer are largely treatable and less severe than melanoma, which presents as an irregular mole.
UV rays from the sun and tanning beds are responsible for most cases of skin cancer. While sun exposure from UV rays may contribute to some degree of skin cancer in African Americans, the genetic makeup plays the largest part in melanoma diagnoses.
“Melanoma shows up in areas that typically are not exposed to the sun, like the toes, tips of the finger or under fingernails and toenails,” said Dr. Tiffany Alexander, dermatologist, ECU Health. “When identified and treated early, most melanoma cases are curable.”
However, melanoma can spread quickly into the blood and to other organs if not found early, and can even be deadly. Knowing that African Americans are more likely to be impacted by advanced melanoma, Dr. Alexander recommends learning the signs and symptoms and taking early action to detect and treat melanoma in its earliest stages.
“African Americans typically present in a more advanced stage because there is not a lot of awareness of melanoma occurring in African Americans, and the perceived risk of melanoma among African Americans is typically low,” said Dr. Alexander. “Many people also neglect to check areas that are not typically exposed to the sun frequently.”
Completing regular self-exams of areas both exposed to the sun and areas not exposed, like fingers and toes can help catch irregularities early. The ABCDEs of melanoma can help in identifying odd or suspicious moles that may need a second look by a dermatologist.
- A: Asymmetric, irregular shape
- B: Borders that are irregular and not round
- C: Color – a mole that is differently colored than other moles
- D: Diameter more than 6 mm in size
- E: Evolving, growing rapidly, a mole that becomes symptomatic
One of the most common misconceptions is that people with darker skin do not get sunburned, according to Dr. Alexander.
“A common myth I hear from my patients is that people with darker skin do not get sunburned,” said Dr. Alexander. “While those with more melanin in their skin have more protection against the sun, I encourage everyone to wear sunscreen with a minimum 30 SPF, no matter skin color.”
Most importantly, Dr. Alexander says, pay attention to your body.
“Get out of the sun if you feel yourself burning,” said Dr. Alexander. “If there is a mole that fits in the ABCDEs of melanoma or a lesion that is not healing or spots that are bleeding, itchy or painful, see a dermatologist.”
Dermatologists provide professional and thorough skin checks and can identify potentially cancerous areas early, when treatment options are great and the cancer is curable. To find a dermatologist near you, please visit ECUHealth.org/dermatology.
ECU Health is proud to announce that the North Carolina Healthcare Association (NCHA) awarded Melanie Porter, administrator of hospital operations, and DeAnna Edwards, manager of hospital operations, the Healthier Communities award for their work in the Statewide Patient Movement Coordination Team. This award recognizes collaborative work by NCHA member organizations to promote health and well-being by addressing an identified community need.
COVID-19 has put a strain on health care systems across the globe and here in North Carolina. Throughout the pandemic, hospitals and health systems have worked tirelessly to advance new approaches to promoting more equitable health outcomes for patients, families and communities. Among these innovations, the Statewide Patient Movement Coordination Team emerged.

The Statewide Patient Movement Coordination Team is a group of individuals at transfer centers across North Carolina who have worked tirelessly during the pandemic to ensure critical patients needing higher levels of care were transferred or those facilities given additional clinical support.
As part of this team, Melanie and DeAnna are both dedicated to living the ECU Health mission of improving the health and well-being of eastern North Carolina. Through their work, they ensure patients have quality care and are connected to the level of care and resources needed.
The Statewide Patient Movement Coordination Team assisted 35 facilities not formally connected with the 13 transfer centers across the state who had critical patients needing higher levels of care.
In total, this team reviewed 765 patient movement requests during the Delta and Omicron surges of COVID-19.
Please join us in recognizing Melanie and DeAnna for representing ECU Health and making a difference in the lives of those we serve.
Leaving a child, senior or pet behind in a car can pose serious danger, even if it’s just for a few minutes.
That was the message of the hot car safety event hosted by Ellen Walston, Injury Prevention Program coordinator at ECU Health Medical Center, along with the Pitt County Health Department and the Martin-Pitt Partnership for Children.
Walston said it’s dangerous for anyone to be left alone in a vehicle because of how quickly they can heat up, but especially for children.

“Children’s bodies heat three to five times more quickly than adults,” Walston said. “They all have a smaller amount of body surface so they can’t cool themselves very quickly. A small child, like the families we’re serving today, they can’t verbalize when they’re thirsty if they’re under a certain age. You really have to be very careful. The message is never leave a child alone in a car, not even for a minute.”
The team had a demonstration with temperature gauges and s’mores roasting in a vehicle on an 80-degree day, one of the coolest days in recent weeks in eastern North Carolina. Despite the cooler than normal temperatures, the interior of the van rose to 90 degrees within 15 minutes, over 100 degrees after an hour, and approached 120 degrees in an hour and a half.
The s’mores demonstration showed how quickly things can literally cook inside of a car when left alone.
“As you see we have this temperature gauge here and just in the last 15 minutes, it’s already gone up 10 degrees,” Walston said. “This is a white car with light interior, and with a dark car and dark interior it can heat the car more quickly.”
Walston noted that there have already been 10 deaths across the country this year from children left alone in cars. In North Carolina, we have seen one this year and another in neighboring Virginia.
She said more than 50 percent of child deaths from hot cars are from children that have been forgotten in vehicles. She said children can be forgotten when routines are broken and leaving something like keys, your cellphone or a briefcase in the backseat next to the child is a safe way to ensure the child is not left alone.
According to Walston, about 17 percent of hot car fatalities are children that are intentionally left behind. She said no amount of time is safe for a child to be left alone, even with windows cracked.
“Many times folks think that, I’m just going into the store for a few minutes, but anything could happen inside, you could become distracted and forget the child,” Walston said. “There is a misnomer that if you crack a window and that will offer some less heat, but that really is a myth. It doesn’t affect the temperature of the car.”
As a rural health care organization, we know there are many challenges to fostering a healthy community. That doesn’t stop ECU Health team members from finding creative solutions to bring health care outside the walls of our hospitals and clinics in eastern North Carolina and into the communities we serve.
KaSheta Jackson, DNP, RN, vice president of Health Equity and Social Impact at ECU Health, and her team developed Community Pop-Ups: A Rural Approach, an innovative health care delivery model implemented as community-based pop-up clinics across eastern North Carolina to address social and economic health care barriers.
This program makes health care both more accessible and approachable by directly providing preventative services, improving health care equity, and offering resources within communities with the greatest need.
Jackson was recognized earlier this year by the American Nurses Association (ANA) and the American Nurses Foundation (the Foundation) as the recipient of the 2022 ANA Innovation Award. The ANA Innovation Awards highlight, recognize and celebrate exemplary nurse-led innovations that improve patient safety and health outcomes. The innovation award also generated a $25,000 grant, which will fund future community health events.
Jackson said nurses are on the leading edge of connecting their fellow community members to health care and should feel empowered to innovate in that space.
“Our innovation has empowered many nurses to think and behave differently with regards to changing health care delivery and where care is delivered,” Jackson said. “By aligning the community and the health care system, we are addressing social, economic, equity, and population health, allowing us to meet our mission of improving the health and well-being of eastern North Carolina.”
Through partnerships with community leaders and other ECU Health team members, these clinics have evolved from solely offering health care screenings to providing COVID-19 testing, vaccinations, mental health resources, access to fresh produce and employment opportunities.
In 2021 alone, Community Pop-Ups provided care to more than 400 community members, identified acute diseases, provided numerous jobs, gave away 500 produce boxes, and delivered 500 health passports in rural locations across eastern North Carolina.
“We are following the model of doing health care on the outside to make health care better on the inside,” Jackson said during a July 2021 community health event in Farmville. “We’re working to address the social determinants of health, offering employment, trying to take care of the need for vaccines, taking health care into communities versus having people come to us – we’re taking services to those that need them.”
As these pop-up events evolve and grow, Jackson hopes they will help create a healthier eastern North Carolina, strengthen ties between community organizations and improve relationships between community members and health care providers.
“I am so excited to see our innovation become reality,” Jackson said. “The advice I would give to any nurse who wants to take their innovations from just an idea to action: be inquisitive, be nosey, ask questions, listen and it will be easy to make it happen.”
This is just one example of how Jackson and her team break down barriers to bring health care to the communities we serve. ECU Health also hosts a myriad of community events including: a foot clinic with Joy Soup Kitchen and Access East, which gives free foot care supplies to diabetic patients who visit the event, over-the-counter medication giveaways and Kids Eat Free with Sodexo, which provides free lunches and afternoon snacks for kids and teens up to age 18.
For more information, visit the Pop-Up Community Health Events page on our website.
Health care workers are well-versed in serving their community, even if that community happens to be an ocean away.
“I’m from Tanzania, east Africa. In a rural village called Taloha,” said Daniel Makoko, behavioral health team member at ECU Health.
After settling in eastern North Carolina, Makoko continued to help improve living conditions in his home village.
“The village has one primary school,” Makoko said. “So these kids use like four classrooms but there are like 270 kids. They share the classroom because it’s not enough. But also the main problem was that the room was leaking when it’s raining.”
So Makoko set about raising money through donations and events like yard sales to put a new roof on the primary school.
“They asked me, ‘What can we do?’ So I told them that if we can get a roof for them, It will be much transformation for the school,” said Makoko.
A transformation in more ways than one, made possible with the help of friends, family and colleagues.
“He’s a great inspiration to me just to see all the things that he has accomplished”, said Tony Dixon, a behavioral health team member at ECU Health. “Between four yard sales and donations from behavioral health services, we were able to raise the four-thousand dollars to get the roof done.”
“I was able to go there and implement the project and we finished the roof and the kids were so happy,” said Makoko.
It’s joy no roof can contain and an example of ECU Health values making a difference half a world away.
“This shows the greatness of the people here and how they are able to respond to the needs of other people across the world,” said Makoko. “I really appreciate it so much.”
Resources
Watch more ECU Health News videos