Kelly Spivey received a call from an ECU Health recruiter during a difficult time of her life.
“I was in a vulnerable situation at home, and I was looking for a way out,” she said. “I cried out to God about what to do. Then the recruiter called me.”
The recruiter invited Kelly to a job fair, citing an application Kelly had filled out. The only catch was Kelly hadn’t filled out an application.
“Then how did your information come across my desk?” the recruiter asked.
“I felt like God was telling me where to go, so I went to the job fair,” Kelly said. “I received three job offers that day. I packed up me and my two boys and moved with nothing. I’ve been here ever since.”

That was in 2012. Kelly began working in the traumatic brain injury (TBI) unit as a care partner, and she loved it.
“I had always felt a calling to work in health care, and in this job, I got to work with a special population of patients. I also met my now-husband, Lee Spivey, who was a charge nurse there.”
When a physical therapy technician announced his retirement from the rehab team, he suggested Kelly apply for his job.
“I interviewed and started working as a tech in 2014,” she said. “I joined the military in 2016, but I stayed at the hospital PRN. Lee and I got married in 2016, and he transferred to [ECU Health] Edgecombe Hospital, but I stayed in Greenville working in rehab, drilling for the National Guard on weekends and serving as the after-school director at my kids’ school.”
Even when the pandemic shut down schools, Kelly still worked PRN at ECU Health Medical Center and in a remote position at the Down East partnership. Over the next few years, Kelly found out she was pregnant, had a miscarriage, left the military, discovered she was pregnant again and supported her husband when he was diagnosed with stage 4 lymphoma and later had a heart attack.
“During all of this, Edgecombe hospital and the whole community supported our family,” Kelly said. “I was able to stay on at work because my team worked with me. They have a special part of my heart,” Kelly said. “It’s been such a roller coaster, but the two hospitals gave us hope.”
In June 2024, Kelly received a call from a friend at ECU Health Edgecombe Hospital asking if she’d like to apply for a community health position.
“I really loved working in rehab, but the manager reminded me community is what I do,” Kelly said. “I prayed on it and applied, and I got the job. I’m so glad I did. It’s truly been a blessing.”
A legacy of service
Community is what Kelly does. In addition to her professional work, she established a community pantry, which she runs out of her own house, in April 2018.
“I was coming home one day with my children, and there was a homeless man on the street,” Kelly said. “My son wanted to give him an oatmeal cake, but the man didn’t want to take it. It was laid on my heart to give people a place they could get what they needed and not feel like they were taking it from someone.”
Kelly cleaned up some old furniture, collected food and toiletries, and announced the pantry on her Facebook account.
“It became a hit – people were using it,” she said.
Now, Kelly said people frequently donate to and take what they need from the pantry.
“People might clean out their closets, or those of a loved one, and drop off clothes,” she said. “Sometimes people drop off one thing and pick up something else. Grandparents come and get snacks for their grandkids, or people get a boxed cake mix for a birthday celebration.”
Kelly cited her parents as inspiration for her passion for service.
“My dad could fix anything outside the house, and my mom could fix things inside,” she shared. “My dad always had a huge garden, and he’d drop off food to people in the neighborhood. My mom could sew, and she made us clothes and even made a wedding dress and all the bridesmaid dresses for a woman who was getting married. She was always that person in the family. When I received the Governor’s Volunteer Award, I drove all the way home to Whiteville to give it to her.”
The “sandwich lady”
In her current role, Kelly was instrumental in bringing the Summer Meal Program to Tarboro. She and her team landed on using Braswell Community Center and Park in Tarboro as the hub for their program.
The Summer Meal Program is a partnership between ECU Health and Sodexo, the ECU Health Foundation and Food Lion Feeds to provide free meals to kids, teens and those with disabilities throughout the summer. Free meals are also offered in Ahoskie, Bethel and Greenville.
“It gave people a place they could play, eat and have access to air conditioning,” Kelly explained. “Seeing kids run up and get something to eat – it took me back to my own days as a single mom. I had a calendar with local restaurants’ ‘kids eat free’ days, and that’s how we ate for a while. It upset me to think of those kids not having something to eat.”

Kelly said now she’s known throughout the community as the “sandwich lady,” but for her, the service is not just about providing a meal.
“We offer healthier options for free, and this opened opportunities to share mental health resources. I’ve helped people sign up for ECU Health Now, and I’ve given them information about support groups. This bridges trust between the hospital and the community.”
Kelly said her passion for service has been fueled by her own experiences, and these are opportunities to give back.
“Everyone is going through something, and we’re not meant to do life alone,” she said. “We truly need each other, and this is my purpose.”
Established in 1979, the North Carolina Governor’s Volunteer Service Award honors the true spirit of volunteerism in individuals and groups who make a significant contribution to their community through volunteer service. Individuals or groups from the public, nonprofit and private sectors may be nominated for this award. This year’s winners include one ECU Health team member, Jennifer Congleton, and two ECU Health Medical Center volunteers, Mattox Piscorik and Deborah Coleman.
Jennifer Congleton
Jennifer Congleton grew up volunteering.
“My family owned small businesses and were connected to our community. We always volunteered and gave back,” she said. “It wasn’t new to me.”

The East Carolina University (ECU) graduate said during her time in college she continued to find many ways to serve others.
“I was the ECU Women’s Residence Council president, I joined the SGA and I was a member of Alpha Kappa Alpha Sorority, Incorporated, where I started a global volunteer experience,” she said. “I had a passion for making a difference in my little part of the world.”
Jennifer initially wanted to work in health care as a nurse, but with her interest in community, she thought it would be a better fit to work in public health.
“I earned my degree in public health, and my graduate degree is in adult education with a concentration in community college systems,” she said. “I felt this bridged the gap between volunteerism and my profession, because I want to do what I can to make our community better.”
While working as the director of admissions for Beaufort County Community College in Washington, North Carolina, Jennifer saw a job listing for a coordinator of allied health education. “I hadn’t thought about working at a hospital, but they wanted someone with an undergraduate degree in public health and a master’s in adult education,” she said. “That was me.”
Jennifer now serves as the director of chaplaincy and volunteer services at the ECU Health Medical Center.
“My current role allows me to help grow volunteers and put them in places where they can find future jobs. We direct them to places where their gifts can be used,” she said. “Volunteers serve as a pipeline. We have many who come here to volunteer and end up working here. We’ve had college students volunteer and then they go to medical school and come back as physicians. Volunteering is a great way to explore jobs while giving back.”
Giving back continues to be a big part of Jennifer’s life. Before her most recent recognition, she was the 2015 Volunteer of the Year at the American Cancer Society’s Hope Lodge, she was elected as the 19th Mid-Atlantic Regional Director of Alpha Kappa Alpha Sorority for 2018 – 2022 and in 2022, she was honored with the Order of the Long Leaf Pine, the highest award for state service granted by the Office of the Governor.
Despite her past recognitions, Jennifer was surprised to learn she had won a Governor’s Volunteer Service Award.
“I had no idea I had been nominated,” she said. “I was shocked. I have been in the working world for almost 40 years, and I thought this was a great way to recognize my career. But you can’t rest on your laurels.”
Mattox Piscorik
Mattox Piscorik began his service at ECU Health as a VolunTeen, first at ECU Health Medical Center and then at ECU Health Beaufort Hospital, where he transported patients, worked in the emergency department and greeted people in the hospital lobby.
Service in health care came naturally to him; Mattox comes from a long line of health care practitioners, including his mother, an ECU Health nurse, and his two brothers, both pursuing careers in health care fields. “We are heavily involved in service in our family,” he said. “We believe in taking care of others as we want to be treated.”
After his work as a VolunTeen, and his graduation from high school this past spring, Mattox joined the cardiovascular intensive care unit (CVICU) in June as an adult volunteer.
“I stock supplies in rooms and make sure all patients and their families are comfortable. The CVICU can be a high-stress environment,” he said. “I also assist with patient transport, and I sometimes help with scanning or faxing to help the nurse manager. I have loved every minute of it.”
Work in the CVICU is even more meaningful to Mattox because his father was once a patient there after having open heart surgery. “To work with some of the same people who cared for him is super special,” he said.
The experience has also inspired Mattox to make a change in his career plans.
“I started off wanting to be an emergency department doctor,” he said. “After being a VolunTeen, I changed my plans and decided to pursue health care administration. But after working on the CVICU, I have decided I’m going to nursing school.”
Mattox is currently attending ECU in the Honors College and plans to apply for nursing school next fall. “The end goal is to get a job in the CVICU,” he shared.
Mattox said he was shocked to learn he’d won a Governor’s Volunteer Service Award.
“I was stunned when I got the email from Chad Tucker,” he said. “I was also honored and humbled to know that my years of hard work and dedication had paid off. I am driven by the belief that small acts of care can lead to big changes, and I’m eager to learn and grow in a field that truly makes an impact.”
Deborah Coleman
Deborah Coleman joined the ECU Health volunteer team with her husband’s and Jennifer Congleton’s encouragement.
“My husband was working as a volunteer before me, and he said I’d enjoy it. Jennifer also kept asking me to volunteer, and I kept telling her no,” Deborah said. “Then one day I changed my mind, and I’ve been doing it ever since. I enjoy it.”
“I met Deborah through my mother,” Jennifer shared. “When I realized Deborah was retired, I told her about the world of volunteering at the medical center and how she could make a difference. Deborah is full of compassion, and we need more like her.”
Deborah works as a patient escort, and she likes meeting different people.
“I take them to different areas of the hospital for screenings or tests, or I take them out after they’re discharged. It’s nice to meet people. Even if they’re grumpy, I tell them, ‘Today is a good day! Smile because God has blessed you to be here.’ I like to make them feel better.”

More than 70 emergency services nurses and physicians from across the ECU Health system came together Oct. 8, for the inaugural Emergency Services Nursing Summit at Eastern AHEC. The daylong event offered a mix of professional development, peer connection and heartfelt recognition for the vital work of emergency department teams.
The summit began with welcoming remarks from Dustin Bass, vice president of emergency services at ECU Health, and Dr. Leigh Patterson, chief of services for emergency medicine at ECU Health Medical Center and chair of emergency medicine at Brody School of Medicine at East Carolina University, setting the tone for a day focused on professional growth and celebrating the contributions of ED nurses.
One of the first sessions addressed imposter syndrome, led by Rachael Smith from the Emergency Nurses Association (ENA), offering insights into overcoming self-doubt in high-pressure environments.

Dr. Trish Baise, chief nursing executive at ECU Health followed with a presentation on The State of Nursing at ECU Health, highlighting current initiatives, challenges and the future direction of nursing within the organization.
The afternoon featured a series of practical and forward-thinking sessions. Theresa Wilson from Stryker shared strategies for pressure injury prevention, helping nurses strengthen patient safety practices. Lori Puthoff from Mednition introduced attendees to AI for Nursing, exploring how artificial intelligence is streamlining workflows in emergency care.
Later, Paige Tyson led an interactive workshop titled, “True Colors”, which helped participants better understand personality styles and how they influence communication and teamwork.
Throughout the day, attendees had opportunities to network, share experiences and build connections across hospitals and disciplines.
“We have EDs in every hospital across the system, but they are all different,” Bass said. “Bringing us together creates opportunities to collaborate, share resources and learn from each other.”
Bass said he hopes the summit helped nurses build relationships with peers and physicians, meet leaders and potential mentors and feel inspired to explore new career paths.
“I also hope they leave with a sense of gratitude for what we’re able to do for patients, feel uplifted and have a renewed sense of purpose,” he added.
The summit not only recognized the dedication of ECU Health’s emergency services teams but also reinforced the organization’s commitment to innovation, collaboration and excellence in patient care.

ECU Health celebrated Wear Pink Day on Oct. 17 to honor those impacted by breast cancer and to raise awareness of the importance of annual screenings. In addition to wearing pink, the Cancer Care team and members of the East Carolina University Women’s Basketball team, including head coach Kim McNeill, handed out pink ribbons and information about breast cancer and 3-D mammograms to ECU Health team members and ECU Health Medical Center visitors.
ECU Health Cancer Care and the ECU Women’s Basketball team work together to share the importance of early detection for breast cancer across the community. For several years, the Women’s Basketball team, assistant coaches and staff, as well as McNeill, have visited ECU Health Medical Center to greet and educate team members and patients.
“Even with their busy season starting, the ECU Women’s Basketball team is committed to spreading this awareness message,” said Phyllis DeAntonio, administrator of ECU Health Cancer Care. “We are extremely grateful for the team’s commitment to ECU Health’s mission, to improve the health and well-being of eastern North Carolina.”

Screenings are important for prevention and early detection. ECU Health offers 3D mammography at 11 locations throughout eastern North Carolina. Key advantages of 3D mammography include:
- Greater detail for improved accuracy
- 40 percent increase in cancer detection
- Locates more invasive, life-threatening tumors
- Better at detecting cancer in dense breast tissue
- Digital images allow doctors in other locations to consult if needed
- Fewer call-backs, resulting in less anxiety
- Patient-friendly design that is more comfortable for all breast sizes
As Breast Cancer Awareness Month continues, make sure you are talking with your health care provider about receiving regular mammograms. Women at higher risk may need to start screening earlier. Learn more about breast cancer and finding a screening location near you by visiting ECU Health’s breast cancer page.
Greenville, NC — Andy Zukowski, chief financial officer of ECU Health, has been recognized by Becker’s Hospital Review as one of 38 Rural Hospital and Health System CFOs to Know in its newly released list. Zukowski, who has served as CFO since 2022, oversees financial operations for both ECU Health and the Brody School of Medicine at East Carolina University.
“It is an honor to be nationally recognized for the work the entire team does at ECU Health,” said Zukowski. “Our goal is to build the national model for high-quality rural academic health care, and being good stewards of our resources is a key component of that. I am proud to work alongside mission-driven individuals who dedicate their time, expertise and energy to meeting the mission of ECU Health by improving the health and well-being of eastern North Carolina.”
Rural hospitals are a lifeline for communities that too often face barriers to convenient, affordable and high-quality care. According to Becker’s, the CFOs featured on the list are the financial architects behind that mission. With expertise in planning and resource management, they strengthen the financial foundation of their hospitals while driving cost-effective, innovative and accessible care. Their leadership ensures that rural communities continue to benefit from up-to-date services and sustainable healthcare delivery.
“Andy brings a mission-focused approach to financial leadership that reflects ECU Health’s broader mission to serve and uplift our communities,” said Dr. Michael Waldrum, CEO of ECU Health and Dean of the Brody School of Medicine.

“As the largest health care provider, employer and medical educator in the region, Andy’s strategic insight helps ensure we remain a strong, sustainable force for health, education and opportunity in rural eastern North Carolina. We’re proud to have Andy helping lead the way.”
Becker’s Hospital Review accepted nominations and curated the list to highlight the outstanding accomplishments of rural hospital CFOs across the country. The full list, which includes individual profiles of each honoree, can be viewed on Becker’s website. Inclusion on the list is not exhaustive nor an endorsement, and individuals cannot pay for placement.
Greenville, NC — ECU Health Chief of Ophthalmology Services Dr. Ann Ostrovsky successfully performed the health system’s first procedures with the Alcon UNITY™ Vitreoretinal Cataract System (VCS), a groundbreaking advancement in ophthalmic surgery that merges cataract and retina capabilities into one integrated platform. ECU Health Medical Center is the first hospital in North Carolina to obtain a UNITY™ VCS.
“As a physician serving eastern North Carolina, it is imperative that we integrate the most advanced surgical technologies into our local care delivery,” said Dr. Ostrovsky. “This technology allows us to offer high-precision ophthalmic procedures, significantly reducing the need for patients to travel long distances. By improving intraoperative stability and reducing energy delivery to ocular tissues, we are enhancing both safety and recovery outcomes while maintaining access to high-quality care close to home.”
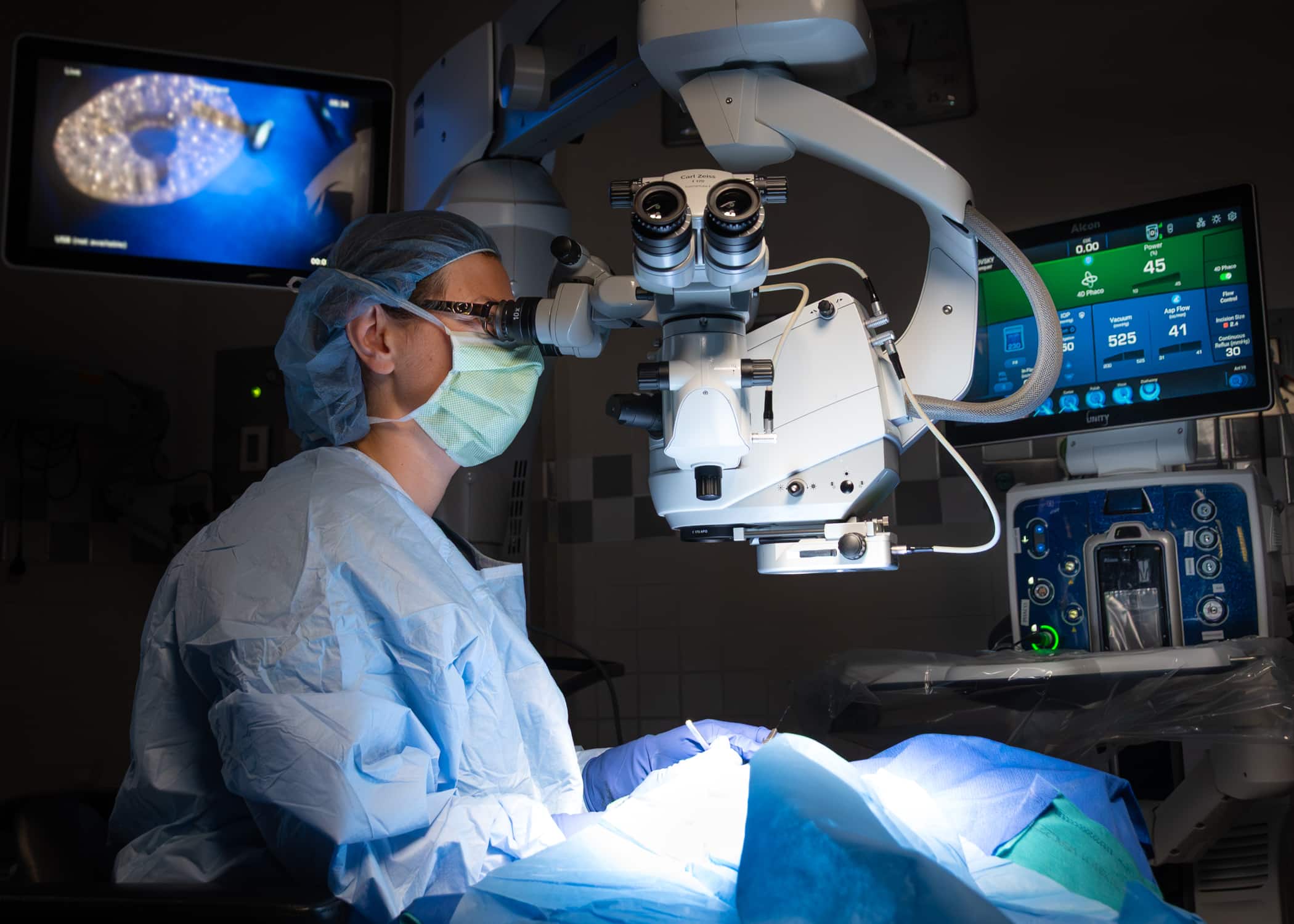
According to Dr. Ostrovsky, the UNITY™ VCS enhances eye stability during procedures, reduces intraocular pressure and minimizes energy use within the eye. These improvements translate into shorter operating times, gentler procedures and faster visual recovery for patients undergoing cataract or retinal surgery. Thanks to these technological advances, patients with advanced cataracts and retinal disease are now experiencing dramatically improved outcomes.
Many cataract surgery patients are achieving excellent vision as early as the day after surgery, an extraordinary leap forward compared to the extended hospital stays and long recoveries that were common just a few decades ago, according to Dr. Ostrovsky. ECU Health’s newly appointed vitreoretinal surgeon, Dr. Peter Jones, will also leverage the UNITY™ VCS to treat complex retinal conditions, including diabetic and rhegmatogenous retinal detachments.
“This milestone reflects ECU Health’s deep commitment to bringing cutting-edge care to the communities we serve,” said Brian Floyd, chief operating officer of ECU Health. “Innovative technologies allow us to deliver world-class treatment without requiring patients to travel far from home. ECU Health is meeting people where they are and ensuring that rural eastern North Carolina has access to high-quality care close to home.”
“This was a calling. I experienced hospice at a young age when my grandfather died from cancer, and I’d seen life end in difficult ways when I worked in the trauma unit. I knew there had to be a better way.”
Nicole Averett, a nurse practitioner at the ECU Health Medical Center, knew from an early age that she wanted to work in palliative care.
Her grandfather was diagnosed with colon cancer and passed away when Nicole was in 7th grade. “He was courageous, and he didn’t want a poor quality of life. At a young age, I witnessed a beautiful death. I spent time with him, I helped care for him and I got to see that people can choose how their final moments can be. That had a lasting impression.”
After a surgery for appendicitis, during which she appreciated and valued her compassionate care, Nicole decided she wanted to work in health care. “I realized I could take care of people who were sick and scared like I was,” she said.
A North Carolina Nurse Scholar scholarship gave her the means to attend ECU, another stepping stone in her path to nursing. “I never even toured ECU, but when I got that scholarship, I decided that’s where I wanted to go.”
After graduation, Nicole joined the surgical intermediate unit, but she knew she wanted to do more. “I wanted to become a nurse practitioner, and I knew I wanted to work in palliative care.”

She attended the University of North Carolina Wilmington and joined the palliative care team in 2014. Now, she helps patients across the hospital and works with a supportive team. “You have to be a compassionate, empathetic person for this line of work,” she said. “We have a lot of fun together and we’re a tight-knit group. Three of my team members have been here more than 10 years.”
Palliative care, while often confused with hospice, does not necessarily mean a patient is dying. “It’s really about living the best you can despite your illness or circumstances,” Nicole said. “The true goal is to help people live the best they can with advanced illnesses. Quality of life can get lost in health care. You need to look at the whole person, and that’s our specialty.”
Nicole said her experience with her grandfather helped her understand that death was a part of life. “We have to deal with it and honor it,” she said. “It’s the norm to not acknowledge terminality, but then you can’t work through things that give you peace.”
Her other grandfather passed away in hospice from Alzheimer’s in his 80s. These experiences showed Nicole what it means to “die well,” and now she’s passionate about making sure everyone knows they have options. “It helped me decide how I wanted to die, but it also made me want to help others understand they have options.”
“How I define dying well isn’t the same for someone else,” she clarified. “I had a patient from Ocracoke who really loved Christmas, and she said being at home with her tree and family brought her joy. Even though it was summer, her family put up her Christmas tree. She didn’t know she could have this joyful experience.”
“A goal of palliative care is to honor a patient’s wishes,” Nicole continued. “Witnessing a peaceful death at home, surrounded by loved ones, really put the itch in my bones to help others. It really is a calling.”
To learn more about palliative care services at ECU Health, visit their website here.
NAGS HEAD, N.C. — October 1, 2025 — Outer Banks Health (OBH) has a new, state-of-the-art mammogram screening machine, Senograph Pristina 3D with Efficiency Suite 2. This advanced screening technology offers higher accuracy in diagnostic performance, especially in dense breast tissue, by using 3D imaging to reduce the overlap of tissues, which can hide abnormalities in 2D scans. With a 40% higher cancer detection rate and the ability to find more invasive, life-threatening tumors, 3D screening mammography offers unmatched clarity and peace of mind. The new Pristina takes images faster than 2D and supports greater patient comfort due to an ergonomic and patient-comfort-forward design that gives patients the option to apply the pressure themselves.
“Outer Banks Health is committed to our community’s health and well-being. That’s why we invest in state-of-the-art technology. We also respond when the community provides feedback on our services. In addition to our new equipment, it is easier than ever to get an appointment for your mammogram, and our waiting room is now warm, welcoming and ready for your next visit,” shared Amy Montgomery, executive director of OBH.

OBH has refined its mammogram scheduling system, creating an additional 30 appointments per week, with plans to increase this number further. The wait time for a mammogram is less than one month, and patients are now able to self-schedule through the MyChart patient portal if they have an order from an ECU Health or OBH provider.
On the day of their mammogram screening appointment, patients also now enjoy upgrades to the mammogram imaging suite. These upgrades were funded by proceeds from the recent Nags Head Links Ladies Driving Fore a Cure Golf Tournament. Thanks to the Nags Head Links Ladies, the mammogram suite now provides an atmosphere that promotes patient comfort. Features such as a gown warmer, a TV, a coffee station, new furniture and artwork, and other cosmetic elements, such as new curtains, painted walls and artificial skylights have all been added to improve the patient experience.
The most likely outcome of a mammography screening is peace of mind that comes from knowing you do not have breast cancer. When breast cancer is detected, Outer Banks Health has the highest quality of care available to help patients navigate the breast cancer journey.
In fact, the Outer Banks Health Breast Care Program has once again been accredited by the National Accreditation Program for Breast Centers of the American College of Surgeons, marking its second recognition since 2022. OBH’s full cancer program has earned Commission on Cancer accreditation three times in a row since 2016. Out of over 1,300 similarly sized hospitals, OBH is the only one in the nation to earn this prestigious designation. OBH has a full team of screening and cancer care specialists ready to help and guide patients every step of the way. OBH is also accredited by the American College of Radiology as a gold standard of medical imaging, as OBH offers the safest and best quality of care possible.
Our high-quality care is evidenced by the fact that OBH has reduced the breast cancer mortality rate in Dare County. When OBH opened in 2002, the county’s breast cancer mortality rate ranked among the highest percentiles statewide. Today, it is among the lowest, at an above-average survival rate. Since OBH’s opening, the detection of life-threatening tumors has shifted dramatically from clinical diagnoses to proactive screenings. Previously, results were primarily discovered in a clinical setting, with only 44% of women having regular screenings. Now, 80% of women in Dare County are learning of their results through proactive screenings, increasing their chances of survival if any life-threatening discoveries are made. This significant decrease in mortality rate is the direct result of OBH’s initiatives, including promoting regular screenings, fundraising for state-of-the-art mammography technology, and fostering a community-wide focus on prevention and well-being.
Further, our high-quality care is available to all. Outer Banks Health offers free screening mammograms to individuals who do not have health insurance. Dare County residents, as well as Hyde, Currituck and Tyrell county residents who work in Dare County, are eligible. The free screenings are made available through the Get Pinked! Program of Outer Banks Health’s Development Council. Since 2011, we have provided more than 2,800 free mammograms.
Breast cancer screening using mammography is recommended to begin at age 40. An order from a provider is needed to schedule a mammogram appointment. Contact your primary care provider or OB/GYN to obtain a mammography order. For more information about screening mammography at Outer Banks Health and to schedule your appointment, call (252) 449-5918. If you need a primary care doctor, call (252) 449-4540 to be connected to an available provider.
Windsor, N.C. – ECU Health Bertie Hospital is proud to announce it has earned an overall hospital quality five-star rating for 2025 from the Centers for Medicare & Medicaid Services (CMS). This recognition places the hospital among the top-performing facilities nationwide and highlights its commitment to delivering compassionate, high-quality care to the communities of eastern North Carolina.
“This five-star rating is a reflection of the exceptional care our team provides every day,” said Brian Harvill, president of ECU Health Bertie Hospital. “This recognition is a testament to our strategic focus on patient-centered care and the connection we share with the community we serve. I am incredibly proud of our team here at ECU Health Bertie Hospital and grateful for the trust our patients place in us.”
The CMS Five-Star Quality Rating System evaluates hospitals based on mortality, safety, readmission, patient experience and timely, effective care.

Ratings are calculated using data hospitals report through several CMS programs and only include measures for which data are available. A rigorous seven-step methodology is used to standardize scores, group measures and assign star ratings based on performance within peer groups. ECU Health Bertie Hospital’s five-star rating reflects its excellence across these measures and its commitment to delivering high-quality, patient-centered care.
“The experience of patients and families is at the heart of safe, highly reliable, human-centered rural health care,” said Dr. Niti Armistead, chief quality and clinical officer, ECU Health. “This CMS five-star patient experience rating at ECU Health Bertie Hospital signifies to us that our patients trust and value our care. It is the result of an intentional focus on creating truly exceptional loving experiences for our patients and their families, and I could not be prouder of the ECU Health Bertie Hospital team.”
ECU Health Bertie Hospital was also recently named one of the top 20 Critical Access Hospitals in the nation for patient satisfaction. A Critical Access Hospital is a classification assigned by CMS to qualifying rural hospitals across the United States. These facilities play a crucial role in enhancing health care accessibility for rural communities by delivering essential medical services and receiving cost-based reimbursement for Medicare-covered treatments.
Clear communication is key when it comes to positive patient experiences and outcomes, and no one knows that better than the Language Access Services team at ECU Health.
“One of the most rewarding aspects of my career as a medical interpreter is that it gives me the opportunity to directly impact the well-being of patients,” said Macaria Aguirre, certified health care interpreter III (Spanish). “Medical interpreters are essential advocates for patients because we play a key role in fostering trust and building strong relationships between patients and health care professionals.”
Betzabe Rodriguez, health care interpreter III (Spanish), says their role goes beyond interpreting word-for-word.
“Interpreting requires conveying meaning, while respecting tone, intent, and cultural context,” she said. “We must interpret faithfully, without adding, omitting or substituting, and adapt to how language really works — it’s not static. Beyond language, we connect values, culture and purpose so providers and patients can truly understand one another.”

Language Access Services team members assist during a wide range of medical events, from explaining diagnoses and prescriptions to supporting families during births, surgeries and emergencies. Their presence helps patients feel safe, valued and understood.
ECU Health’s first ASL resident, Jordan Satchell, takes pride in her ability to advocate for patients who use sign language to communicate. She says she’s here to help ensure nothing gets lost in translation, literally.
“When patients or staff are misunderstood, it can lead to serious errors or delays in care,” said Satchell. “I can step in immediately, adapt to fast-changing situations, and make sure both patients and providers understand one another fully. That kind of access and clarity is not just convenient, it’s essential,” she said.
Supporting patients during uncertain times, team members often form close connections with those they assist. Satchell recalled one patient transferred to ECU Health after being diagnosed with cancer while on vacation. The patient had spent a week at a previous facility communicating only through writing.
“The moment I entered her room, she lit up and said, ‘I’m so happy to see you!’” Satchell said. “We had never met, but we built a strong connection during her month here. Before she returned to her home state, she told me how much she had seen my confidence and skills grow. That feedback meant so much to me. I’ll always remember her.”
Satchell says working with patients through the ASL interpreter residency program also provides the opportunity to strengthen her skill.
“No two people sign or use ASL in the same way. There’s always something new to learn,” she said.
ECU Health currently has a total of 24 Spanish interpreters and two ASL interpreters to meet the needs across the system. Other languages are available through a virtual service, connecting patients and providers to interpreters for more than 200 languages. A translator is also available virtually for written word.
Demand for Language Access Services continues to grow. Patients requiring interpreters throughout the system increased from 9,000 in 2022 to more than 12,000 this past year. That figure multiplies when accounting for accompanying family members and caregivers who also need language support.
Rodriguez said she hopes the program continues to expand to meet the needs of the region.
“I hope we keep building a system where language and cultural barriers no longer stand in the way of health, safety or dignity,” said Rodriguez.
As ECU Health celebrates its Language Access Services team this week, be sure to thank them for the vital role they play in delivering positive patient experiences and outcomes.
At ECU Health Medical Center, Spanish interpreters are available in person 24/7. The team can be reached at 252-874-4470, option 3 for ASL; option 4 for Spanish. You can also contact the team at [email protected].



