Dr. Audy Whitman wears a few hats: he is the program director for the Rural Family Medicine Residency program at the Brody School of Medicine at East Carolina University; an assistant clinical professor in the Brody School of Medicine’s department of family medicine; and physician at ECU Wound Healing clinic. Balancing multiple roles and responsibilities is nothing new to the eastern North Carolina native, whose resume also includes a stint as a farmer.
“I am from a small town called Seven Springs, N.C. It was and is a farming community,” Dr. Whitman said. “Growing up, I worked on my grandparent’s farm. I worked in chicken houses and hog houses; I’ve cropped tobacco; I’ve driven tractors for harvest.”
It was that hard work, in part, that motivated him to pursue a career in medicine.
“Farming is backbreaking and grueling work,” he said. “There’s no more powerful motivator in the universe to pursue higher education than standing in a tobacco field in later summer, with 99% humidity, no shade and 100-degree temperatures. Your hands are soaked in tobacco gum, and the nicotine is soaking into your skin, so you feel nauseated all the time. I’m not saying it’s not good work to do, but it motivated me to do other things.”
Another inspiration came from his small town’s family physician, Dr. Paul Bennett.
“He was a Med-Peds (internal medicine and pediatrics) doctor by training, but he did everything a family medicine physician would do in a rural community,” Dr. Whitman explained. “He took me under his wing and talked to me about a future career in medicine.”
After high school, Dr. Whitman found himself at East Carolina University where he completed two undergraduate degrees in biology and anthropology and a master’s in cellular biology. Prior to his career in medicine, Dr. Whitman was a regulatory specialist for the North Carolina Department of Agriculture and Consumer Services, in the agency’s Food and Drug Protection division, as well as a contract inspector for the U.S. Department of Agriculture and the U.S. Food and Drug Administration (FDA). In his FDA role, he earned a special citation from the U.S. FDA Commissioner for his work on a nationwide food recall.
“I also worked for the North Carolina Community College System as a pre-health science instructor at Lenoir Community College in Kinston,” he said. “I got tired of my students calling me ‘doctor’ when I hadn’t earned that moniker, so I got serious about the idea of going into medicine. Dr. Bennett told me I should go into family practice, so he helped put me on that trajectory.”
Dr. Whitman attended the Brody School of Medicine, and in 2017, he joined the Department of Family Medicine faculty. In 2020, he was made the program director for the Rural Family Medicine Residency program.
“My detail-oriented work ethic and my ties to rural eastern North Carolina are why I was asked to head up that program,” Dr. Whitman said.
Those ties to eastern North Carolina included experiencing hurricanes that significantly impacted his hometown.
“People not from around here won’t remember hurricanes Fran or Floyd, but I recall vividly that my town flooded very severely over the years from hurricanes, and especially from those two,” he said“I recall sitting on my back deck and realizing our community was an island, and people couldn’t go anywhere.”
He also realized that the elderly and sick had nowhere to go to seek medical care.
“It provided a buy-in for me that we need doctors in these rural communities for events like this when you’re truly isolated and need boots on the ground,” Dr. Whitman said. “That experience played a role in getting the rural program up and running and productive.”
Now, Dr. Whitman is proud of the Rural Family Medicine program’s growth and its impact on rural communities like Seven Springs.

“I help train the next generation of family physicians to care for the people of eastern North Carolina and play an active role in designing systems to address health care disparities in our rural communities,” he said. “It’s fulfilling and rewarding work, and it’s an honor I don’t take lightly.”
Because of his efforts, resident physicians and graduates effect meaningful change across the region.
“When you have a patient come in for a 15-minute appointment, they often have a laundry list of other things to address because this is the one trip to the doctor they get this month,” Dr. Whitman explained. “In these cases, I think about my grandma. How would I want her treated? With these rural program residents, they are taking care of my flesh and blood.”
Without the various roles he’s held over his career, Dr. Whitman said he wouldn’t be the clinician, educator or advocate he is today.
“I’ve had both blue-collar and white-collar jobs. I’ve worked in the unforgiving elements of brutal eastern North Carolina summer heat and in positions where the health and safety of our population were dependent on the actions of me and my colleagues,” he said. “I have worked jobs in which I had the honor to educate and provide eastern North Carolinians the tools to broaden their minds and their career prospects. Through all these experiences, I have gained an appreciation for meeting people where they are and treating people with respect. They have made me who I am and compel me to do the work I do today.”
Dr. John Catanzaro, professor and chief of the Division of Cardiology at the Brody School of Medicine at East Carolina University and director of the East Carolina Heart Institute at ECU Health Medical Center, was recently honored with the prestigious Dr. John “Jack” Rose Distinguished Professorship, recognizing his significant contributions to improving health care delivery, excellence in clinical medicine, administration and academic advancement, including formation of the first Clinical Cardiac Electrophysiology Fellowship at ECU Health.
The Rose Professorship, established by ECU Health and East Carolina University through the ECU Health Foundation and state funds, honors Dr. Rose, a renowned cardiologist and professor. This endowed title supports the director of the East Carolina Heart Institute recognizes Dr. Rose’s exceptional contributions to cardiology and medical humanitarian work. Dr. Rose, who joined ECU Health in 1982 and the Brody School of Medicine in 1990, is celebrated for his dedication to patient care, teaching, and community service. Recipients of this professorship are expected to embody his ideals and passion for teaching, inspiring future generations of medical professionals.
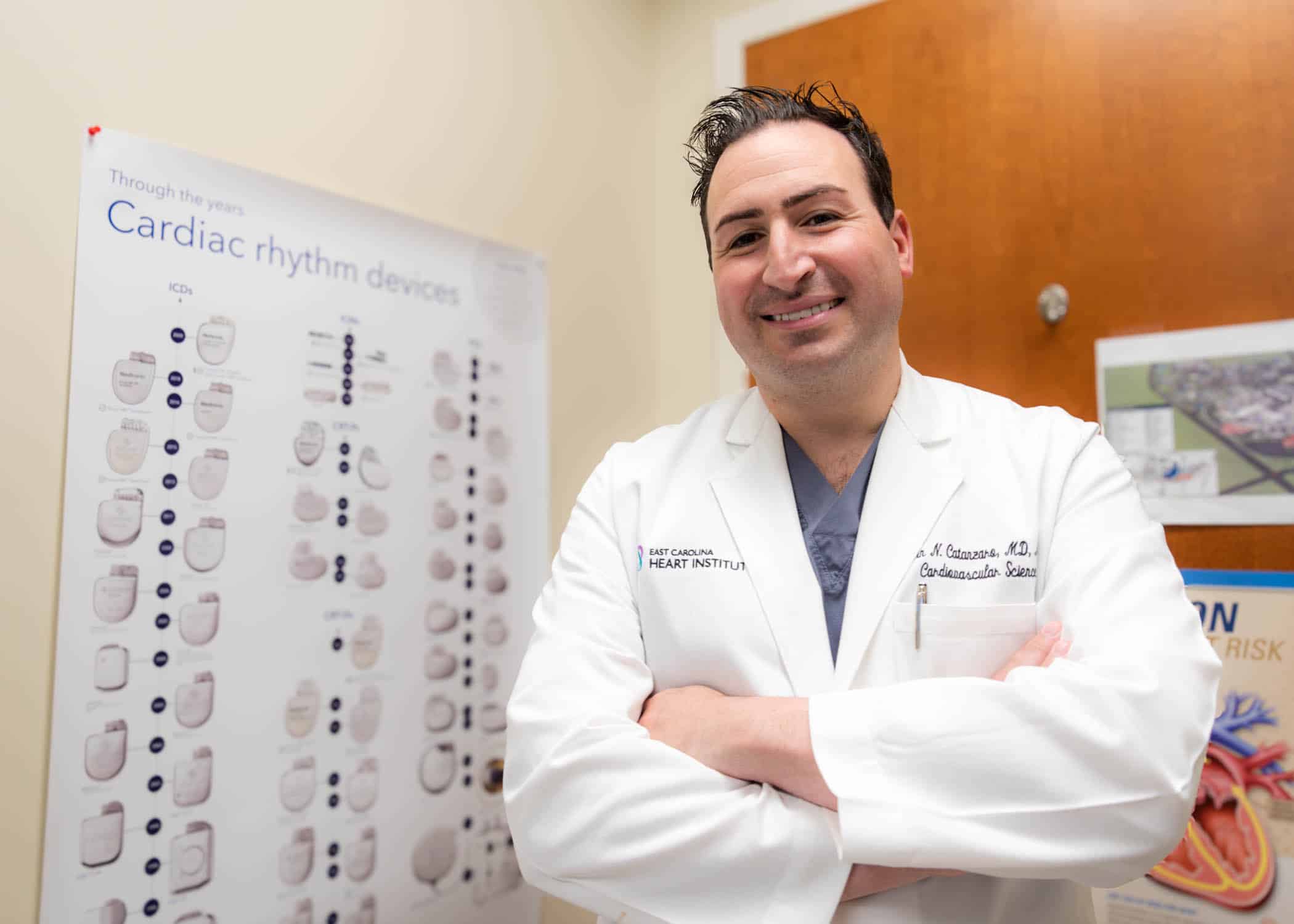
“It’s an honor to be named to the Rose Professorship,” said Dr. Catanzaro. “This title not only recognizes Dr. Jack Rose’s work and legacy, which is focused on humanitarianism and the humanistic qualities of medicine, but it also allows me to highlight and continue his remarkable contributions. As program director, I perform hands-on teaching with trainees during cardiac procedures as well as teach didactic sessions. My primary role is to train the next generation of electrophysiologists to increase access to the patients of eastern North Carolina while maintaining a high standard of excellence in administration and leadership. This professorship is an opportunity to advance Dr. Rose’s legacy of teaching, administration and leadership, ensuring that his impact endures in these areas.”
Dr. Catanzaro completed his Doctor of Medicine with distinction in research at SUNY Downstate Medical Center, followed by an internal medicine residency and cardiovascular disease fellowship at North Shore University Hospital and a clinical cardiac electrophysiology fellowship at The Johns Hopkins Hospital. He also holds an MBA from the University of Florida. He is a Fellow of the American College of Cardiology, Heart Rhythm Society European Heart Rhythm Society and European Society of Cardiology. Dr. Catanzaro is actively involved with the Heart Rhythm Society’s Atrial Fibrillation Stroke Prevention Task Force and serves as vice chair of their Quality Improvement Committee. Nationally recognized for his work, Dr. Catanzaro has delivered invited presentations and chaired panels in the U.S., France, Italy, Germany, England, Romania and more. He also performed recorded procedures for the Heart Rhythm Society Scientific Sessions.
Dr. Catanzaro wanted to transition to an administrative role to broaden his impact beyond individual patients to the entire region and the cardiology division.
“We thought he was the best person for the future of cardiology,” said Dr. Mark Iannettoni, W. Randolph Chitwood, Jr, MD, Distinguished Chair in Cardiovascular Sciences, Brody School of Medicine at ECU and chief, Cardiovascular Service Line at the East Carolina Heart Institute at ECU Health Medical Center. “Dr. Catanzaro possesses a highly entrepreneurial spirit, bringing significant innovation to ECU Health. He has developed new techniques and devices in electrophysiology, advancing our capabilities in device management and patient care.”
The Rose Professorship comes with an endowment, managed by the university, to support ongoing and future initiatives in medical education and innovation. The endowment provides approximately $64,000 annually to advance the cardiology division’s educational and innovative efforts, supporting activities such as purchasing educational equipment, facilitating attendance at conferences, and other educational pursuits.
“The professorship facilitates innovation within the field by providing the necessary funding for new initiatives, such as introducing new devices,” said Dr. Catanzaro. “The goal is to use a certain amount of the endowment each year to support these innovations and to produce more trained physicians for the region. This helps establish our institution as a center of excellence and makes our advancements known.”
Dr. Catanzaro utilized part of the endowment to establish a two-year Electrophysiology Fellowship, admitting one fellow per year, starting this year. Electrophysiologists treat heart rhythm disorders and heart failure with electric devices inserted into the heart. As part of the fellowship, doctors will learn about pacemakers, defibrillators, implantation, ablations, leadless pacemakers, and left atrial appendage closure devices.
“This was one of the fastest fellowships from concept to establishment that we’ve ever done, which just goes to show you how much drive Dr. Catanzaro has,” said Dr. Herb Garrison, former associate dean for ECU’s Brody School of Medicine Graduate Medical Education. “It typically takes two to three years to establish a new residency or fellowship, and we did this in less than a year. That was a record time. And part of that had to do with Dr. Catanzaro and Alyson Riddick, who did an excellent job putting the application together.”
Dr. Jan Lopes is the first fellow in the Electrophysiology Fellowship at ECU Health. He learned about the new program through his cardiology fellowship leader in El Paso, Texas, and decided to join the fellowship because of Dr. Catanzaro’s strong vision for the program.
“Dr. Catanzaro’s enthusiasm for the program and education, along with the opportunity to shape the program for future fellows, attracted me to the fellowship,” said Dr. Lopes. “Despite being a new program, it feels well-established and highly developed. I feel incredibly supported in my role and am receiving top-tier training that rivals what is offered at major medical centers nationwide. We are utilizing cutting-edge technology and performing the latest procedures here at the medical center.”
Training doctors like Dr. Lopes with the latest technology and procedures is important for the future of health care. The need for well-trained electrophysiologists is increasing across the nation and here in eastern North Carolina, according to Dr. Garrison.

“The incidence of arrhythmias, along with the need for pacemakers and defibrillators, is rising as the population ages, making it a critical area of focus,” said Dr. Garrison. “Establishing residencies and fellowships serves two main purposes: recruiting top-tier faculty and creating a pipeline of skilled electrophysiologists. Faculty are attracted to institutions with trainees, and enhancing our program with excellent faculty was a strategic move by Dr. Catanzaro. This initiative ensures we have the necessary capability and qualified physicians to meet the growing demand for electrophysiology services.”
With the increasing demand for physicians and electrophysiologists trained to treat rural patients, Dr. Catanzaro’s efforts at ECU Health is paying off in the form of improved recruitment efforts.
“Dr. Catanzaro has successfully attracted numerous cardiologists,” said Dr. Iannettoni. “He has excelled at developing divisions within the cardiology department and navigating the integration of academia and medicine. His efforts have resulted in many of our graduates choosing to stay with us, which is a significant benefit of our program. We’re proud to retain our own trainees, ensuring continuity and excellence in our team.”
Each summer, teenagers from across eastern North Carolina dedicate a portion of their summer to serve their community at ECU Health hospitals across the region.
The VolunTeen Program is designed to teach students ages 15-17 the value of community service and to provide experiences that foster growth and maturity. The program runs from June to August and volunteers serve at least one shift per week at the hospital.
At ECU Health Medical Center, 122 teens completed 4,717 hours of service across 39 departments this summer. Sara Tingen, volunteer services coordinator at ECU Health Medical Center, said this year was very successful and they hosted their largest group of VolunTeens since the onset of the COVID-19 pandemic.
While the volunteers serve in many roles across the hospital, Tingen said patient transporting from one area of the hospital to another is one of the most important tasks.

“The (ECU Health) Cancer Center alone can see 400 people in one day,” Tingen said. “That’s a lot of time it would take for a nurse or other team members to transport a patient, they rely heavily on our transport volunteers. They can just pick up the phone, say, ‘Hey, I need this person to go here to there.’ And it’s done, they can move on to caring for their next patient. We’re proud to be a smiling face and someone patients can connect with while we help them get around.”
Emily Anthony recently finished her third summer in the VolunTeen Program, where she spent her time escorting patients, assisting the Volunteer Services team on projects and serving as a leader for other VolunTeens.
She said her favorite part of the VolunTeen Program is talking to patients and team members while also making connections with her fellow VolunTeens. Emily is entering her senior year of high school and wants to pursue health care.
“It’s really great to get experience in health care, because I want to do something in health care, maybe a nurse,” she said. “The first summer, I just thought it would be a good experience to do the VolunTeen Program but I just loved working in the hospital. I worked in a unit the first summer with all the nurses and I just loved it.”
Christopher Latimer is entering his sophomore year of high school and said he had a great experience in his first year as a VolunTeen. He’s already decided he’ll join again next summer.
He said he’s had an interest in nursing and getting first-hand experience working alongside nurses has helped him understand the day-to-day work of a nurse in a hospital setting.
“I was on 2 South most of the time and I worked in the Cancer Center as well,” Christopher said. “They were both good experiences. I was going around, asking patients questions and seeing if I could help them in any way. I helped the care partners, seeing if I could help out the nurses with anything, really. I’m thinking about nursing and I’m going to also try and do different areas the next time I VolunTeen to see more and just kind of see my options in health care.”

Chad Tucker, director of Volunteer Services at ECU Health Medical Center, said Christopher’s experience is exactly what the program hopes to give back to the local students who are spending their time serving their community.
“This program is an investment in our future,” Tucker said. “A lot of these students are going into college and they get a chance to see the hospital first hand. It’s so rewarding when you see former VolunTeens who are in medical school, or they’re nurses here, they’re respiratory therapists, they are in various capacities and they attribute part of their foundation to the VolunTeen Program. These young people are able to help team members and the patients we serve, but it also gives them help in their careers.”
The program also offers Leadership Sessions for VolunTeens, which gives them a chance to see unique areas of the health system and opportunities for skill development. In one session, the group visited the EastCare helipad, learned about the team, got to look around the inside of a helicopter and even saw a landing.
In another session, the Human Resources and Workforce Development team worked on resume building and shared interview tips with the VolunTeens.
“We have quite a few seniors who are coming up on college applications so if they’re interviewing for jobs or interviewing for scholarships, it just gives them a good perspective on how to navigate possibly their first interview as a young adult,” Tingen said.
We’re proud to support the VolunTeen Program at ECU Health Medical Center and select ECU Health Community Hospitals and we’re grateful for the teen who step up each summer to help us serve eastern North Carolina.
To learn more about the VolunTeen Program and other volunteer opportunities at ECU Health, visit ECUHealth.org/Volunteers.
Windsor, N.C. – Wallace Nelson, RPh, has been awarded the Bowl of Hygeia Award given by the North Carolina Association of Pharmacists (NCAP). Established in 1958, the Bowl of Hygeia Award is sponsored by the American Pharmacists Association Foundation and the National Alliance of State Pharmacy Associations. The award recognizes one pharmacist from each state annually for their exceptional record of community leadership. NCAP Executive Director Penny Shelton praised Wallace, noting that he has “walked the talk his entire career finding ways to serve and give back at extraordinarily high levels.”
Nelson has been employed by ECU Health Bertie Hospital and ECU Health Chowan Hospital for over 40 years, with 37 years in management. His professional career started in retail pharmacy before joining ECU Health where he continues to serve both hospital locations.
“I am very humbled to have been selected to receive the Bowl of Hygeia from NCAP and NASPA. I view giving back to our community and state as opportunities to serve others and strive to make things better for all, something that I treasure being a part of,” Nelson said.

ECU Health Pharmacy manager, Shelli Simmons, PharmD, stated, “ECU Health Bertie and Chowan Hospitals are thankful for Wallace’s dedication to our healthcare system. He is very deserving of this prestigious award, and it recognizes his commitment not only to our patients, but also our communities. I am very honored to work alongside with Wallace.”
A Perquimans County native and graduate of the College of the Albemarle and The University of North Carolina at Chapel Hill. On a local level, Nelson served on the Perquimans County Board of Education for four terms and then the voters of Perquimans County elected him to serve as a County Commissioner, a position he holds today. He is also actively involved in the North Carolina Association of County Commissioners where he will be installed as President Elect in August 2024 and President in 2025. Past appointments by a number of North Carolina Governors include the College of Albemarle Board of Trustees, North Carolina Marine Industrial Authority, several Governor’s Councils, Institutes and Legislative Study Commissions. Fifteen years ago, the pharmacists of North Carolina elected him to serve on the North Carolina Board of Pharmacy, a position he holds today.
Previously, Nelson received the Order of the Long Leaf Pine by Governor Beverly Perdue, which is North Carolina’s highest honor for those who have made significant contributions to their state and local communities. During his service on the Board of Education he received the Raleigh Dingman Award, the highest honor given to a school board member, presented annually by the North Carolina School Boards Association.
It is no secret that medical residency can be stressful. The three-to-seven years doctors spend as a resident are jam packed with experiences that prepare them for a career in the fast-paced environment of health care.
For ECU Health Medical Center residents, that stress is left behind the moment they walk into the brand-new Resident Well-Being Zone – a space intentionally designed to ensure they can take time to relax, reflect and focus on their own well-being.
Located on the 6th floor the Eddie and Jo Allison Smith Cancer Center at ECU Health Medical Center, the Resident Well-Being Zone is filled with all the essentials a resident may need: exercise equipment, charting space, healthy snacks, coffee, even a ping-pong table and more. It is thoughtfully designed with experience in-mind, according to ECU Health Chief Well-Being Officer Dr. Christina Bowen.

“Residency has a quite a bit of emotional labor,” said Dr. Bowen. “Learning at an incredibly rapid pace and being exposed to cases that pull at your heart strings can be stressful. How do you deal with those challenges and manage those emotions and still be prepared to provide high-quality care? We believe that having a space for residents to decompress, even if for 5 or 10 minutes during their day can help them to continue to focus on their learning and care of patients as well as support their personal well-being. Many times they will be able to walk up to the Well-Being Zone and connect with a fellow resident who is having a similar experience which is a concept called common humanity which we know supports self-compassion. Residents’ compassion for themselves helps them as they share compassion with their patients and colleagues helping to create a culture where they can thrive.”
The Resident Well-Being Zone opened in June but it is a space that’s more than five years in the making. The idea was sparked when ECU Health CEO and Brody School of Medicine at East Carolina University Dean Dr. Michael Waldrum saw an article about a similar effort at another health system. With a grant from the ECU Health Foundation and partnership from the General Medical Education Well-Being Committee, the Resident Well-Being Zone was launched to immediate fanfare, with residents flocking to the ping-pong table.
“We’re all excited about the Well-Being Zone and thankful to ECU Health and the GME Well-Being Committee for prioritizing our wellness while on the wards,” said Dr. Natalie Malpass, a third-year family medicine resident at ECU Health Medical Center. “It’s great to have a space of our own where we can re-center and re-charge, even if only for a few minutes. Between the inviting couches, the ping pong table, coffee bar, and workstation for when the pager inevitably goes off, the committee really thought of everything.”
The opening of the Resident Well-Being Zone is a culmination of years of planning, but Dr. Bowen said this is only the beginning. She is planning to build on the initial success by adding well-being pop up events throughout the year.
“This Well-Being Zone is an example of the amazing collaboration we have here at ECU Health,” said Dr. Bowen. “We were able to identify a need and partner with many teams across the organization to make this unique space possible. We are grateful for our residents and we hope they feel their well-being is supported so they can continue to do the important work of caring for patients and furthering their knowledge of compassionate medicine.”
Greenville, N.C. – East Carolina University’s College of Nursing and ECU Health are launching an Adult Gerontology Acute Care Nurse Practitioner program, a new graduate-level certificate program that will prepare more specialized nurse practitioners in acute care settings across the state.
“We have a lot of nurse practitioners in North Carolina who are doing amazing work to care for patients in ICUs and other very demanding care sites, we also want to expand the knowledge, skills and abilities of current practitioners because the need is so high and the shortage of providers is so great,” said Dr. Julie Linder, chair of the Advanced Nursing Practice and Education department. “This new program will provide the didactic and clinical experiences necessary to meet the needs of our patient populations.”
According to the American Association of Nurse Practitioners, only 6.1% of nurse practitioners specialize in adult gerontology acute care.

The aging population is growing nationally, along with an ongoing shortage of health care workers. The collaboration between the College of Nursing and ECU Health bolsters the health care workforce in eastern North Carolina, enhances health outcomes and increases access to specialized care for older adults in these communities.
“ECU Health values its strong partnership with ECU and the College of Nursing, especially in addressing the national health care workforce shortage,” said Pam Rudisill, vice president of nursing excellence at ECU Health. “Our success as an academic health system relies on bridging clinical and academic excellence to provide high-quality care to eastern North Carolina. Eastern North Carolina depends on collaborative solutions from institutions like ECU Health and ECU to meet the needs and improve the health and well-being of our region.”
ECU Health’s Chief Nursing Office will support their employees by offering tuition reimbursement as a commitment to support the certificate program and help employees advance their education and skills.
The first cohort of ECU’s Adult Gerontology Acute Care Nurse Practitioner certificate program will begin classes in Spring 2025. Students who complete course requirements on the recommended plan of study should graduate in May 2026. Upon graduation, these students will be eligible to take a specialty exam to become certified as Adult Gerontology Acute Care Nurse Practitioners.
The application deadline for that first cohort is Dec. 15, 2024, and applicants can find application requirements and procedures, along with required courses in the curriculum, here.
The certificate program is a post-master’s program, which means applicants must already be recognized as an advance practice nurse. The education students will receive will provide them with the skills to work in acute care settings. ECU offers pre-requisite courses if prospective students have not already completed them.
“We invite prospective students to contact us in the event they need pre-requisite courses prior to beginning their core class work,” Linder said.
ECU’s College of Nursing and ECU Health previously developed pathways for the development of the future of nursing care in eastern North Carolina with the establishment of an academic-practice partnership, seeded by a $1.5 million investment from ECU Health over five years. This investment has provided the ECU College of Nursing with the opportunity to hire faculty, staff, and purchase resources to support students in the Adult Gerontology Acute Care Nurse Practitioner certificate program.
The first cohort will comprise approximately 12 students, with a minimum of six seats dedicated to ECU Health employees and other slots open to applicants interested in advancing their career in critical care.
ECU will join three other nursing programs in North Carolina to offer the AGACNP certification.
Greenville, N.C. – After six years with ECU Health, including serving as president of ECU Health North Hospital since August 2020, Jason Harrell has announced his retirement effective Aug. 8, 2024. ECU Health has begun a national search for the next president of ECU Health North Hospital. Dennis Campbell II, DHA, RN, NEA-BC, will serve as interim president of ECU Health North Hospital in addition to his current role as president of ECU Health Beaufort Hospital.

Jason Harrell
“On behalf of ECU Health, I would like to thank Jason for his service and dedication to advancing our mission over the years,” said Van Smith, president, ECU Health Community Hospitals. “Jason has had a distinguished 40-year career in health care, and we are grateful for his service to ECU Health. During his time at ECU Health North, Jason’s leadership, collaboration and focus on the priorities of access, quality, experience and safety have been unwavering. ECU Health North Hospital team members, patients and the community have benefitted from Jason’s leadership accomplishments.”
Campbell, II will serve at ECU Health North on an interim basis until the national search is completed. He has been with the health system for four years, previously serving as ECU Health Beaufort’s vice president of Patient Care Services before taking on the role of president in September 2023.

Dennis Campbell II
During his time at ECU Health Beaufort, Campbell, II has prioritized developing relationships with important stakeholders and partners in the area including Beaufort Community College and ECU, exemplifying his dedication to investing in the future of academic health care in eastern North Carolina.
“Dennis’s leadership skills and deep understating of the needs of our team members and the communities we serve in eastern North Carolina will be invaluable assets to ensure the stability and ongoing success of ECU Health North Hospital during this time of transition,” Smith said. “I appreciate Dennis’s willingness to serve the system in this capacity.”
As an academic health system, ECU Health serves as both a rural care delivery organization and a training ground for health care providers and support services team members.
While resident physicians and nurses come to mind as the most obvious roles that blend the clinical and academic environments, a new resident track is helping bridge an important need for patients across eastern North Carolina who are Deaf or Hard of Hearing: the ECU Health American Sign Language (ASL) Residency program.
Launched in April, the ASL Interpreter Residency program was born from the demand for more skilled ASL medical interpreters. The program is designed to help increase the number of ASL interpreters available to patients across ECU Health’s system, in both hospitals and clinics, as well as train the next generation of interpreters for a career in the medical field.
More than 500,000 people throughout the United States use ASL to communicate as their native language, making ASL the third most common language in the United States, after English and Spanish, according to the Commission on the Deaf and Hard of Hearing.

“There is a massive need for ASL interpreters in health care both nationally and locally,” said ECU Health ASL coordinator Reid Barnes, who designed the program. “When we looked at this need in the lens of our role as an academic health system, it made sense to model something similar to the physician resident experience.”
Residents in the program join with a two-year commitment where they focus on skill development and clinical interpreting during their first year, with close supervision in the clinical setting. The second year of the program incorporates both hospital and clinical work while also assisting with ongoing educational efforts.
Barnes, ECU Health’s only full-time ASL interpreter, works with up to 6 or 7 patients on any given day, often times spread across the health system’s 29 county service area, so the demand is obvious. What is less obvious, however, is the process behind becoming a skilled medical ASL interpreter.
A licensed or certified ASL interpreter does not receive a specialized certificate in medicine. ASL interpreters undergo rigorous testing to ensure they have generalized competencies for a multitude of interpreting settings. However, the decision to specialize in any setting is left to the individual interpreter. Specialization often involves an extensive combination of targeted workshops and firsthand experience. As a result, it is often difficult for newer interpreters to safely gain firsthand experience.
All of these factors, Barnes said, inspired the creation of the ECU Health ASL Interpreter Residency program.
“Health care should always be provided in a patient’s native language,” said Barnes. “Imagine what your health care experience would feel like if you couldn’t communicate with your doctors and nurses in your primary language? For the Deaf and Hard of Hearing community, that is a very real reality. We can now expand our services, improve patient experiences and be a true training ground for skilled medical ASL interpreters.”
Jordan Satchell is the first ever resident in the ECU Health ASL Interpreter Residency program. Having served as an experience coordinator in ECU Health Medical Center’s emergency department, she has a close understanding of the important role ECU Health serves as the flagship health system in eastern North Carolina.
“Returning to ECU Health as the first ASL Interpreter Resident has been a rewarding experience in many different ways,” said Satchell. “You never truly ‘arrive’ when it comes to interpreting, so this program has allowed me to build my skills and improve my knowledge about health care. The patients I work with have already helped me become a better interpreter, and I can only hope to continue serving them, learning their needs, breaking down communication barriers, while also being a resource to the next incoming resident.”
Barnes said Satchell will help chart the future of the program, as the two work together to closely examine the needs of the patient population while tailoring the program’s design to ensure it provides the best resident experience possible.

OUTER BANKS, N.C., July 24, 2024 — Outer Banks Health and Dare County Department of Health & Human Services have joined forces with Blue Zones, the global leader in longevity research and community well-being transformation, to launch Blue Zones Ignite™ Outer Banks.
Blue Zones uses an evidence-based, environmental approach to making healthy choices easier where they live and spend most of their time. Blue Zones will work with Outer Banks Health, the County, and other community leaders to conduct an in-depth feasibility assessment to determine how to make it a healthier place to live, work, and thrive. Together with the community, the Blue Zones team will assess readiness and build a plan for change.
The launch of Blue Zones Ignite is a dream come true for Christina Bowen, MD, Outer Banks Health Center for Healthy Living Medical Director, and ECU Health Chief Well-being Officer.

“We know that 20% of health and longevity is tied to genetics; while 80% is tied to where and how we live. Blue Zones Ignite Outer Banks is going to inspire us to celebrate and promote our strong sense of community while we find ways to make it even easier to eat healthy foods, move naturally and connect with our purpose – just a few of the ways we’ll continue to enhance our well-being and make this an even better place to live and work,” shared Dr. Bowen.
The Blue Zones Approach
Blue Zones employs a proven solution in collaboration with communities to help people live better and longer lives. The company’s work is based on research and principles developed by National Geographic Fellow and New York Times bestselling author Dan Buettner, who identified the cultures of the world – or blue zones regions – with the healthiest, longest-living populations.
The Blue Zones approach focuses on the single largest determinant of health: the place we live. Instead of focusing solely on individual behavior change, Blue Zones helps communities make permanent and semi-permanent changes to policies, systems, streets, surroundings, and social networks so it’s easier for residents to eat wisely, move naturally, and connect more with others as they move throughout their day. By improving the Life Radius®—the area close to home where most Americans spend 90% of their lives—Blue Zones transformations have been able to move the needle dramatically in improving overall population health and well-being. Communities that have participated in the Blue Zone’s Ignite project have seen double-digit drops in obesity and smoking rates, economic investment in downtown corridors, grant funding awards to support policies and programs to improve health equity, and measurable savings in healthcare costs.
“Together, Outer Banks Health and Dare County Health and Human Services are steadfast in our shared mission to enhance the health and well-being of all residents, so that they can live a happy, healthy and long life,” said Dr. Sheila Davies, Director Health & Human Services.
Ben Leedle, CEO of Blue Zones and Co-founder of Blue Zones Project, said: “We are excited to partner with forward-thinking leaders in the joint effort of improving well-being in the Outer Banks. That improvement, at the community level, leads to healthier and happier residents, better and more productive workforces and student bodies, and a more vibrant economy. We are excited to collaborate to create a transformation plan that can generate lasting positive change and ignite a community-wide movement towards sustained well-being.”
The Blue Zones expert team will connect with Outer Banks leaders and organizations to begin immediate work assessing the strengths, needs, and challenges that residents are facing today. Blue Zones will then create a policy-focused transformation plan that, once implemented, can drive widespread improvements in well-being, reductions in healthcare costs, and improve economic vitality in the region.
Greenville, NC — Andy Zukowski, ECU Health chief financial officer, was recently honored by Becker’s Hospital Review as one of 36 Rural Hospital CFOs to Know. Zukowski has served as CFO since 2022 and oversees the financial operations at both ECU Health and the Brody School of Medicine at East Carolina University.

Andy Zukowski, ECU Health chief financial officer
“It’s an honor to be nationally recognized for the work we do here at ECU Health,” said Zukowski. “Our goal at ECU Health is to build the national model for high-quality rural academic health care and being good stewards with our resources is a key component of that. I am proud to work alongside mission-driven individuals who commit their time, expertise and energy to serving the people of rural eastern North Carolina.”
Rural hospitals are an essential component of today’s health care environment, dedicated to serving populations that often encounter obstacles to convenient, quality and affordable care. These institutions play a critical role in ensuring healthcare access for underserved communities. The CFOs highlighted on the list are instrumental in ensuring the financial health of their organizations. Applying their expertise in financial planning, these executives help bring cost effective, innovative, up-to-date and accessible healthcare to their communities.
“Andy’s passion for serving others and mission-focused mindset align with ECU Health’s mission to improve the health and well-being of eastern North Carolina,” said Dr. Michael Waldrum, CEO of ECU Health and Dean of the Brody School of Medicine. “As the largest health care provider, employer and medical educator in the region, ECU Health has a unique role to play in the communities we serve – and Andy recognizes that this depends on the organization’s sustainability. ECU Health is proud to help lead the way in creating jobs and encouraging economic growth to help improve the rural communities we serve, many of which experience socioeconomic distress and health disparities.”
Becker’s is delighted to feature these accomplished leaders, who are critical to the successes of their respective organizations. The Becker’s Hospital Review editorial team accepted nominations for this list and curated it to highlight the fantastic accomplishments of rural hospital CFOs.